Uterine fibroids are a common gynecological condition affecting women of reproductive age. Clinical manifestations vary depending on the size, number, and anatomical location of the fibroid nodules.
What is uterine fibroid disease? Can uterine fibroids be effectively treated? Join Hong Ngoc General Hospital in exploring key clinical aspects and management considerations related to uterine fibroids in the article below.
Clinical manifestations of uterine fibroids
Uterine fibroids, also known as leiomyomas, are benign tumors arising within the uterus. These lesions originate from smooth muscle cells of the myometrium and are strongly influenced by hormonal imbalance, particularly estrogen and progesterone.
Based on their anatomical location within the uterus, uterine fibroids are classified into different subtypes, including submucosal, intramural, and subserosal fibroids. Clinical symptoms vary depending on the size, number, and location of the fibroid nodules.
The most common clinical manifestations of uterine fibroids may include:
- A sensation of pelvic heaviness or lower abdominal pain and pressure.
- Menstrual disturbances, including menorrhagia, prolonged menstrual bleeding, and irregular menstrual cycles.
- Lower back pain resulting from compression of the lumbar nerves by an enlarged fibroid mass.
- Increased urinary frequency or difficulty controlling urination. Large fibroids may exert pressure on adjacent structures such as the bladder or urethra, leading to urinary retention, urgency, stress incontinence, or overflow incontinence.
- Dyspareunia, which may be accompanied by postcoital bleeding.
- Abdominal enlargement or abnormal increase in abdominal girth.
The aforementioned symptoms, when occurring in isolation, are often mistaken for urinary tract disorders or musculoskeletal conditions. Consequently, many patients delay seeking medical evaluation until the manifestations become more severe, which may complicate management and limit optimal treatment outcomes.
Complications associated with uterine fibroids
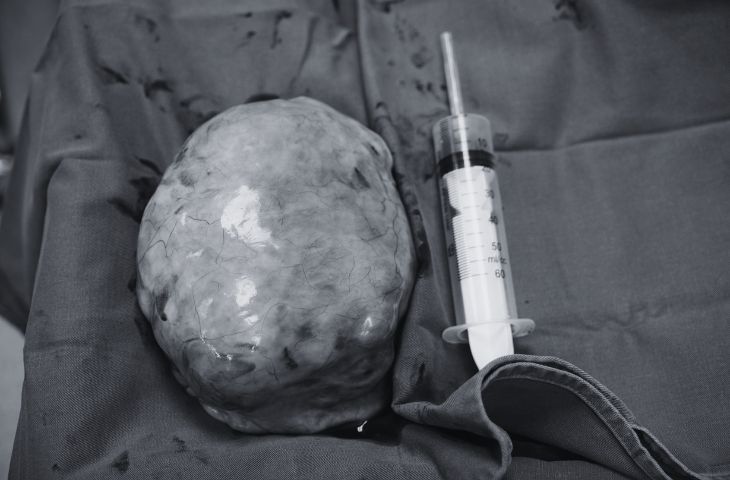
In the early stages, when fibroid nodules remain small, uterine fibroids are often asymptomatic and generally not life threatening. However, as the tumors progressively enlarge, they may give rise to significant complications that adversely affect overall health and, in severe cases, may pose serious risks to the patient’s well being.
Torsion of subserosal fibroids
Subserosal fibroids develop on the outer surface of the uterus beneath the serosal layer. These lesions are often pedunculated with a long stalk, making them susceptible to torsion. Torsion of a fibroid can present as acute abdomen with severe abdominal pain, syncope, nausea, and vomiting, constituting a gynecological emergency that may threaten the patient’s life if not promptly managed.
Infection of fibroid tissue
Infectious complications are more commonly associated with submucosal fibroids, which are anatomically closer to the endometrial cavity and more vulnerable to ascending bacterial invasion. Infected fibroids may lead to endometritis or salpingitis. Clinical manifestations can include high fever, foul smelling vaginal discharge, pelvic pain, and purulent yellow green discharge.
Infertility and adverse pregnancy outcomes
Uterine fibroids are recognized as a contributing factor to infertility and subfertility, particularly when large fibroids interfere with embryo implantation or distort the uterine cavity. In pregnant patients, fibroids may increase the risk of malpresentation, threatened miscarriage, preterm labor, and other obstetric complications.
Additionally, fibroids may obstruct the birth canal, making vaginal delivery difficult and increasing the likelihood of cesarean section.
Reader may also be interested in:
- Are night sweats during pregnancy dangerous? 7 ways to reduce night sweats during pregnancy
- How does chickenpox during pregnancy affect the pregnancy?
- 5 signs of gestational diabetes that pregnant women should pay attention to
Anemia
Hormonal imbalance associated with uterine fibroids frequently leads to menorrhagia or prolonged menstrual bleeding. Chronic excessive blood loss may result in iron deficiency anemia. If not adequately managed with rest and nutritional supplementation, severe anemia can cause dizziness, hemodynamic instability, or even cardiovascular compromise.
Malignant transformation
Most uterine fibroids are benign, and malignant transformation into leiomyosarcoma is rare. Nevertheless, regular gynecological examination every six months is recommended to monitor disease progression and detect potential complications at an early stage.
Patients are advised to undergo reproductive health screening at reputable obstetrics and gynecology centers. To schedule a consultation with leading obstetrics and gynecology specialists in Vietnam, please contact our hotline at 0886 621 046 or complete the registration form below.
How are uterine fibroids diagnosed?
Clinical pelvic examination
In patients with uterine fibroids, the uterus may be enlarged, irregular in contour, and mobile upon bimanual pelvic examination. These features can often be palpated during gynecological assessment. In cases of large fibroid masses, abdominal distension may be visible on inspection, sometimes resembling a pregnancy beyond 12 weeks of gestation.
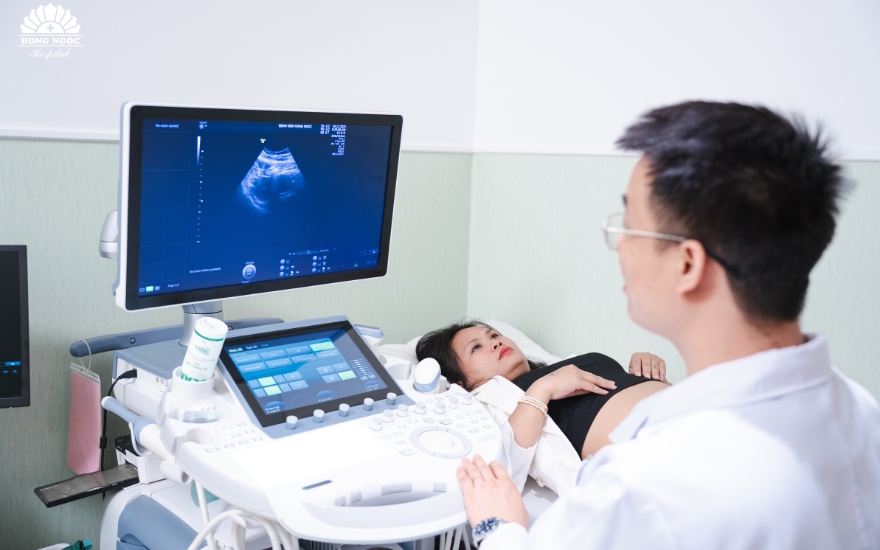
Ultrasonography
With advancements in medical imaging technology, ultrasonography plays a central role in the detection of uterine fibroids, including small, asymptomatic nodules that have not yet caused complications. Transvaginal ultrasound and saline infusion sonohysterography are commonly performed to provide detailed visualization of the uterine cavity and accurately determine the size, number, and anatomical location of fibroid lesions.
Magnetic resonance imaging
When ultrasonography, including saline infusion sonohysterography, does not provide sufficient diagnostic clarity, magnetic resonance imaging serves as a highly effective modality. MRI allows detailed evaluation of fibroid characteristics, including anatomical location, size, number, and relationship to surrounding pelvic structures.
MRI produces high resolution, high contrast images of the uterus, enabling comprehensive assessment of disease extent and severity. In most cases, MRI findings provide sufficient diagnostic information without the need for additional imaging. In patients with atypical features or when deeper evaluation is required, contrast enhanced MRI may be performed to further characterize the lesion.
Management of uterine fibroids
Asymptomatic uterine fibroids generally do not require immediate intervention. In such cases, patients are advised to undergo periodic gynecological evaluation every three months to monitor fibroid growth and assess for the development of symptoms or complications. Timely intervention can be initiated if there is evidence of tumor progression.
For symptomatic fibroids or those associated with complications, two principal treatment modalities are currently employed: medical therapy and surgical management.
Medical therapy for uterine fibroids
Several pharmacologic agents are used in the management of uterine fibroids. The two principal categories include:
- Estrogen suppressive agents: These medications inhibit the stimulatory effect of estrogen on fibroid growth and are commonly prescribed to control abnormal uterine bleeding. Potential adverse effects may include weight gain, mood disturbances such as depression, and irregular uterine bleeding. As these are prescription medications, they must be used strictly under medical supervision.
- Hormone modulating agents: This group includes medications that reduce circulating levels of estrogen and progesterone, thereby contributing to fibroid shrinkage and improvement of anemia related to excessive menstrual bleeding. These agents are often administered preoperatively to decrease uterine and fibroid size and to minimize intraoperative blood loss.
Surgical management of uterine fibroids
Surgical removal of fibroids is typically indicated in patients with large tumor size or in cases where medical therapy has failed to achieve adequate clinical response.
The commonly performed procedures include:
- Myomectomy: Surgical excision of fibroid nodules while preserving the uterus. This procedure is often performed via laparoscopic surgery or hysteroscopy, depending on the size and anatomical location of the fibroid.
- Hysterectomy: Surgical removal of the uterus, which may be performed laparoscopically, via the vaginal route, or through an open abdominal approach, depending on clinical indications and patient specific factors.
In order to minimize the risk of recurrence, patients who no longer desire future fertility are often advised to undergo total or subtotal hysterectomy. This definitive surgical approach provides more comprehensive disease control and significantly reduces the likelihood of fibroid recurrence.
Where to seek evaluation and treatment for uterine fibroids
When undergoing evaluation and management for gynecological conditions in general, and uterine fibroids in particular, women are advised to choose reputable and specialized healthcare facilities.
The Obstetrics and Gynecology Department at Hong Ngoc General Hospital is a trusted destination for comprehensive gynecologic care. The department has successfully performed numerous surgeries for large uterine fibroids, delivering favorable clinical outcomes while preserving patient safety and quality of life. Hong Ngoc remains committed to providing evidence based, patient centered care that supports women’s reproductive health and overall well being.
Hong Ngoc General Hospital is comprehensively equipped with advanced medical infrastructure, including state of the art ultrasound systems such as 2D, 3D, and 4D ultrasonography, color Doppler imaging, and the latest generation Voluson E10 platform. The hospital brings together leading obstetrics and gynecology specialists with extensive clinical expertise, ensuring accurate diagnosis and the development of optimal, individualized treatment pathways.
In addition, patients are assured absolute privacy during consultation and treatment under a dedicated one physician–one nurse care model. All personal and medical information is strictly protected in accordance with patient confidentiality standards.
Note: The information provided in this article by Hong Ngoc General Hospital is intended for reference purposes only and does not replace professional medical diagnosis or treatment. For an accurate assessment of any medical condition, patients are advised to visit reputable healthcare facilities for direct clinical evaluation and appropriate treatment consultation by qualified physicians.











