External hemorrhoids are not life threatening; however, they can significantly impact a patient’s health and quality of life. Each stage of the disease requires different management approaches. Early detection and timely treatment are key factors in achieving optimal outcomes and complete symptom resolution.
What are the stages of external hemorrhoids? Let us explore in the following article.
What are external hemorrhoids?
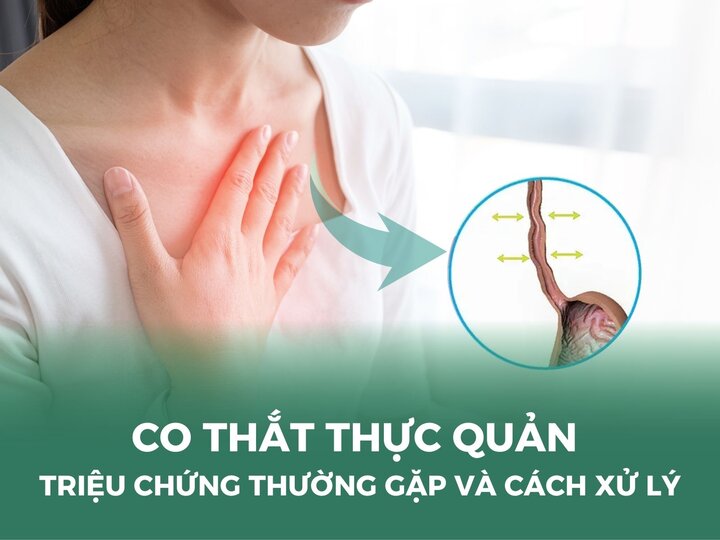
External hemorrhoids are characterized by abnormal dilation of the venous plexus located below the dentate line in the anorectal region, leading to the formation of hemorrhoidal masses.
Unlike internal hemorrhoids, which develop silently within the rectum and are often detected only through endoscopic examination, external hemorrhoids are easily recognizable. Patients may be able to see or palpate the hemorrhoidal masses directly.
In the early stage, external hemorrhoids are typically small, resembling a pea sized, pink lesion, usually painless and without bleeding, though mild itching or irritation may occur. As the condition progresses, the hemorrhoidal masses may enlarge, potentially leading to thrombosis, edema, pain, and bleeding.
The etiological factors of external hemorrhoids are similar to those of hemorrhoidal disease in general, including:
- Prolonged standing or sitting and a sedentary lifestyle, commonly seen in occupations such as drivers, office workers, or security personnel.
- Chronic constipation, leading to excessive straining during defecation.
- Diarrhea, which may increase pressure and irritation in the anorectal region.
- A low fiber diet, frequent consumption of spicy foods, and inadequate fluid intake.
- Underlying conditions that increase intra abdominal pressure, such as irritable bowel syndrome or anorectal tumors.
- Pregnancy and the postpartum period.
If not adequately treated, external hemorrhoids may lead to complications such as anorectal inflammation, anemia due to chronic bleeding, and in severe cases, may be associated with more serious colorectal conditions, significantly impacting overall health and quality of life.
Stages of external hemorrhoids and stage specific management
Unlike internal hemorrhoids, which are classified into four grades, external hemorrhoids are typically categorized based on disease progression into the following stages:
Stage 1: External hemorrhoidal masses are visible or palpable outside the anal verge. At this stage, they are typically painless and non bleeding, though mild discomfort, itching, or a foreign body sensation may occur. This is the earliest and most treatable stage, and prompt medical evaluation allows for effective, often complete resolution with conservative management.
Stage 2: The hemorrhoidal masses enlarge and become more prominent, often associated with dilated and tortuous veins. Patients may experience pain, discomfort, and bleeding during defecation. Poor hygiene may predispose to local infection. Complications such as thrombosis or strangulation may occur if untreated. Management at this stage is usually conservative, including topical agents, oral medications, suppositories, and lifestyle modifications to reduce inflammation and prevent progression.
Stage 3: Hemorrhoidal masses become significantly enlarged, potentially causing partial obstruction of the anal canal. Patients frequently experience severe pain and bright red bleeding during defecation. In advanced cases, complications such as anemia, anal fissures, and secondary infection may develop. Persistent discharge may lead to pruritus ani and unpleasant odor, increasing the risk of local inflammation if hygiene is inadequate.
Management of stage 3 external hemorrhoids depends on the severity of the condition in each individual patient.
In mild cases without significant impact on overall health, conservative treatment with topical agents combined with oral medications may be sufficient to control symptoms.
However, in cases where complications arise or symptoms significantly affect quality of life, minimally invasive procedures or surgical interventions may be indicated, particularly when medical therapy fails to achieve adequate clinical improvement.
Stage 4: This represents the most advanced and severe stage of external hemorrhoidal disease. Hemorrhoidal masses become markedly enlarged, edematous, inflamed, and may ulcerate, leading to persistent pruritus and discomfort.
If not appropriately managed, patients often experience continuous pain, which is exacerbated by prolonged sitting, standing, or ambulation due to friction with clothing. In addition, rectal bleeding during defecation may become more severe, presenting as spurting or continuous dripping of blood.
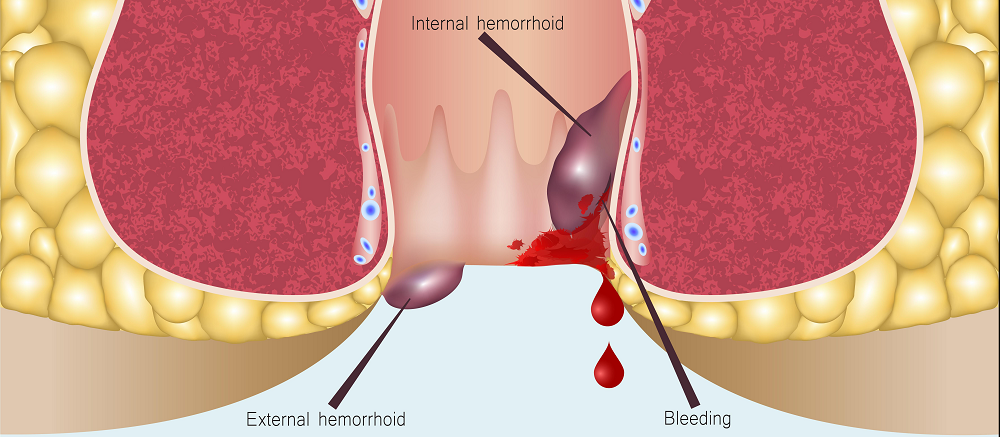
In patients with stage 4 external hemorrhoids, conservative medical therapy is typically limited to symptomatic relief and temporary disease control.
Therefore, definitive management often requires surgical intervention, including techniques such as laser coagulation, rubber band ligation, sclerotherapy, hemorrhoidectomy, or stapled hemorrhoidopexy (Longo procedure), depending on clinical indications and patient condition.
Notes on stage based management of external hemorrhoids
Conservative (medical) treatment
For patients with stage 1 and stage 2 external hemorrhoids, most cases can be effectively managed with conservative therapy, including oral medications, topical agents, and rectal suppositories, combined with appropriate dietary and lifestyle modifications, as follows:
- Increase intake of fiber rich foods, including fruits, vegetables, and whole grains.
- Supplement collagen rich foods such as salmon, tuna, and seaweed.
- Maintain adequate daily hydration.
- Engage in regular physical activity, with low impact exercises such as walking, swimming, or gentle fitness routines.
- Avoid prolonged sitting or standing; take short breaks to walk after every hour of sitting.
- Use a donut cushion when prolonged sitting is required.
- Establish a regular bowel habit by defecating at a fixed time each day to promote optimal gastrointestinal function and prevent constipation.
- Maintain proper anal hygiene after defecation using wet wipes or soft cotton to minimize friction and irritation.
In addition, commonly indicated conservative treatment options include:
- Topical agents containing witch hazel extract or hydrocortisone to reduce inflammation, pruritus, and local irritation.
- Medications regulating bowel function, including agents for constipation or diarrhea, as well as venoactive drugs that enhance venous tone, improve vascular integrity, and provide anti inflammatory effects.
- Rectal suppositories and ointments, applied locally to protect the mucosa overlying hemorrhoidal tissue and facilitate smoother stool passage.
- Analgesics such as ibuprofen, acetaminophen, or aspirin for pain relief (to be used under medical guidance).
- Cold compresses applied to the anal region using ice wrapped in a soft cloth to reduce edema and pain.
- Hypertonic saline ice packs, which may be used in cases of thrombosed external hemorrhoids to alleviate swelling and discomfort.
Patients should be advised that, prior to initiating any pharmacological treatment for external hemorrhoids, it is essential to seek evaluation at a reputable healthcare facility. Consultation with a qualified specialist ensures accurate diagnosis, appropriate therapeutic guidance, and effective management, thereby optimizing treatment outcomes and minimizing unnecessary costs.
Laser hemorrhoidectomy
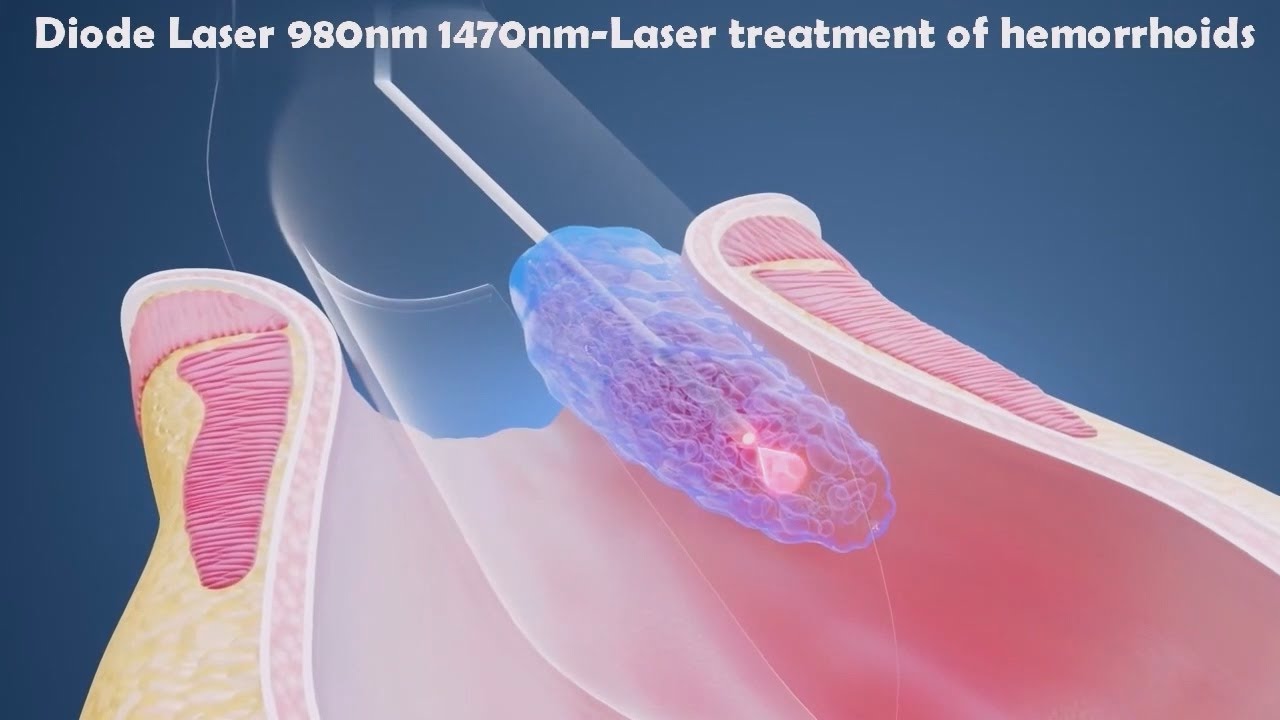
For patients with mild to moderate external hemorrhoids (stages 1, 2, and 3), laser treatment is considered a modern, safe, and highly effective therapeutic option. This technique does not involve conventional surgical excision; instead, it utilizes high energy laser technology to directly target the hemorrhoidal plexus at its origin.
Laser hemorrhoidectomy works by delivering focused thermal energy to coagulate and obliterate the vascular supply feeding the hemorrhoidal tissue. As a result, the hemorrhoidal mass undergoes shrinkage and fibrosis over time.
During the procedure, a micro laser probe (approximately 1.5 mm in diameter) is precisely applied to the hemorrhoidal tissue. The laser energy selectively destroys the feeding vessels without damaging surrounding structures. Consequently, this method is regarded as minimally invasive, with high safety, preservation of the anatomical and physiological integrity of the anal canal, and a reduced risk of postoperative functional impairment.
Reader may also be interested in:
- Signs of external hemorrhoids – when should you seek medical attention?
- What are external hemorrhoids? What is the most effective and safe approach to the management of external hemorrhoids?
- Etiology of external hemorrhoids and effective preventive strategies
Advantages of laser hemorrhoidectomy
- High therapeutic efficacy: Laser hemorrhoidectomy achieves a success rate exceeding 90%, particularly when appropriately indicated for bleeding hemorrhoids at stages 1, 2, and 3, as well as small sized hemorrhoidal masses, under the expertise of specialized clinicians.
- Safe and minimally invasive: The laser energy precisely targets the hemorrhoidal tissue and submucosal vascular plexus without affecting surrounding structures. This allows optimal preservation of the anal sphincter anatomy, physiological function, neural integrity, and anorectal mucosa.
- Rapid recovery: Patients are typically able to ambulate normally within approximately 5 hours post procedure, reflecting minimal tissue trauma and expedited recovery.
- Cost effectiveness: Faster postoperative recovery reduces hospitalization time and overall treatment costs, making this technique economically advantageous.
Other surgical treatment options for external hemorrhoids
For patients with stage 3 and stage 4 external hemorrhoids presenting with complications such as infection, edema, enlarged hemorrhoidal masses, thrombosis causing acute vascular obstruction, significant bleeding, severe pain, persistent discharge, or ulceration, surgical intervention is often indicated. Common techniques include:
- Doppler guided hemorrhoidal artery ligation (DG HAL): This technique utilizes Doppler ultrasound to identify and ligate the arterial supply to the hemorrhoidal plexus, thereby reducing blood flow. Deprivation of blood supply leads to shrinkage and eventual regression of the hemorrhoidal tissue.
- Minimally invasive techniques (radiofrequency or electrocoagulation): These methods do not involve conventional surgical excision. High frequency energy is applied to generate ionic activity, directly targeting dilated hemorrhoidal vessels. Enlarged hemorrhoidal masses may subsequently be excised using electrocautery. This approach minimizes bleeding, reduces postoperative pain, accelerates recovery, lowers recurrence rates, and preserves the integrity of the anorectal mucosa.
- Stapled hemorrhoidopexy (PPH procedure): This technique removes and repositions prolapsed hemorrhoidal tissue above the dentate line, followed by mucosal suturing to restore normal anatomy. It is associated with less postoperative pain, high safety, reduced complication rates, and faster recovery compared to conventional surgery.
- However, if not performed with appropriate technique and expertise, these procedures may be associated with complications such as anal stenosis, constipation, urinary retention, postoperative bleeding, and a risk of recurrence.
- Milligan Morgan hemorrhoidectomy: This is a conventional surgical technique that allows complete excision of hemorrhoidal tissue. The procedure involves ligation and removal of hemorrhoidal masses, followed by preservation or suturing of mucocutaneous bridges to protect the anal canal lining. This approach helps minimize damage to the anoderm while ensuring effective and definitive removal of hemorrhoids.
In addition, clinicians strongly advise that patients with external hemorrhoids should not self medicate. Instead, patients should seek evaluation by qualified healthcare professionals and strictly adhere to prescribed treatment regimens, including dosage and duration, in order to avoid inappropriate drug use or prolonged misuse that may lead to adverse effects.
Furthermore, in cases requiring surgical intervention, patients should attend reputable medical institutions with experienced colorectal specialists. Proper assessment and individualized treatment planning are essential to ensure optimal outcomes, minimize pain, and reduce the risk of perioperative and postoperative complications.
Where to seek effective and reliable treatment for external hemorrhoids?
With the principle of delivering the right treatment for the right condition, Hong Ngoc General Hospital has become a trusted destination for thousands of patients seeking hemorrhoid treatment, offering:
- Accurate diagnosis and definitive treatment delivered by a team of highly qualified and experienced specialists, including: Assoc. Prof. Dr. Nguyen Xuan Hung – Former Director of the Colorectal and Perineal Surgery Center, Viet Duc University Hospital; Vice President of the Vietnam Society of Coloproctology; Member of the French Society for Colorectal and Anal Diseases; Dr. Pham Van Cuong (MD, PhD, Specialist II) – Nearly 40 years of experience; Member of the Vietnam Society of Endoscopic and General Surgery; Dr. Cu Trung Kien (MD, MSc) – Advanced training in gastrointestinal surgery in Hong Kong; Former physician at Bach Mai Hospital; Deputy Head of the Department of Gastrointestinal Surgery, Hong Ngoc General Hospital; Dr. Bach Phuc Huy (MD, Specialist I) – Over 15 years of experience; Head of the Gastrointestinal Surgery Unit, Hong Ngoc – Phuc Truong Minh.
- Painless hemorrhoid surgery with a comprehensive perioperative pain management protocol (pre intra and postoperative) developed by Dr. Nguyen Thi Thu Ba (MD, MSc), who completed advanced residency training in France. A highly skilled anesthesia team ensures continuous monitoring throughout the procedure.
- Proactive pain prevention strategy: Patients undergo thorough pre anesthetic assessment, continuous intraoperative monitoring, and early pain control before symptom onset.
- Advanced surgical techniques targeting non pain sensitive zones, minimizing tissue trauma and preserving anorectal function.
- 24/7 dedicated patient care team providing attentive support throughout hospitalization.
- Spacious, well equipped inpatient facilities designed to meet international hospital hospitality standards.

For detailed consultation, please contact:
Specialist appointment hotline: 0911 908 856 Hemorrhoid surgery consultation hotline: 0949 646 556
Note: The information provided by Hong Ngoc General Hospital is for reference purposes only and does not replace professional medical diagnosis or treatment. For an accurate assessment of your condition, patients are advised to visit reputable healthcare facilities for direct examination and appropriate therapeutic guidance from qualified physicians.
Follow the official fanpage of Hong Ngoc General Hospital for more useful health information.