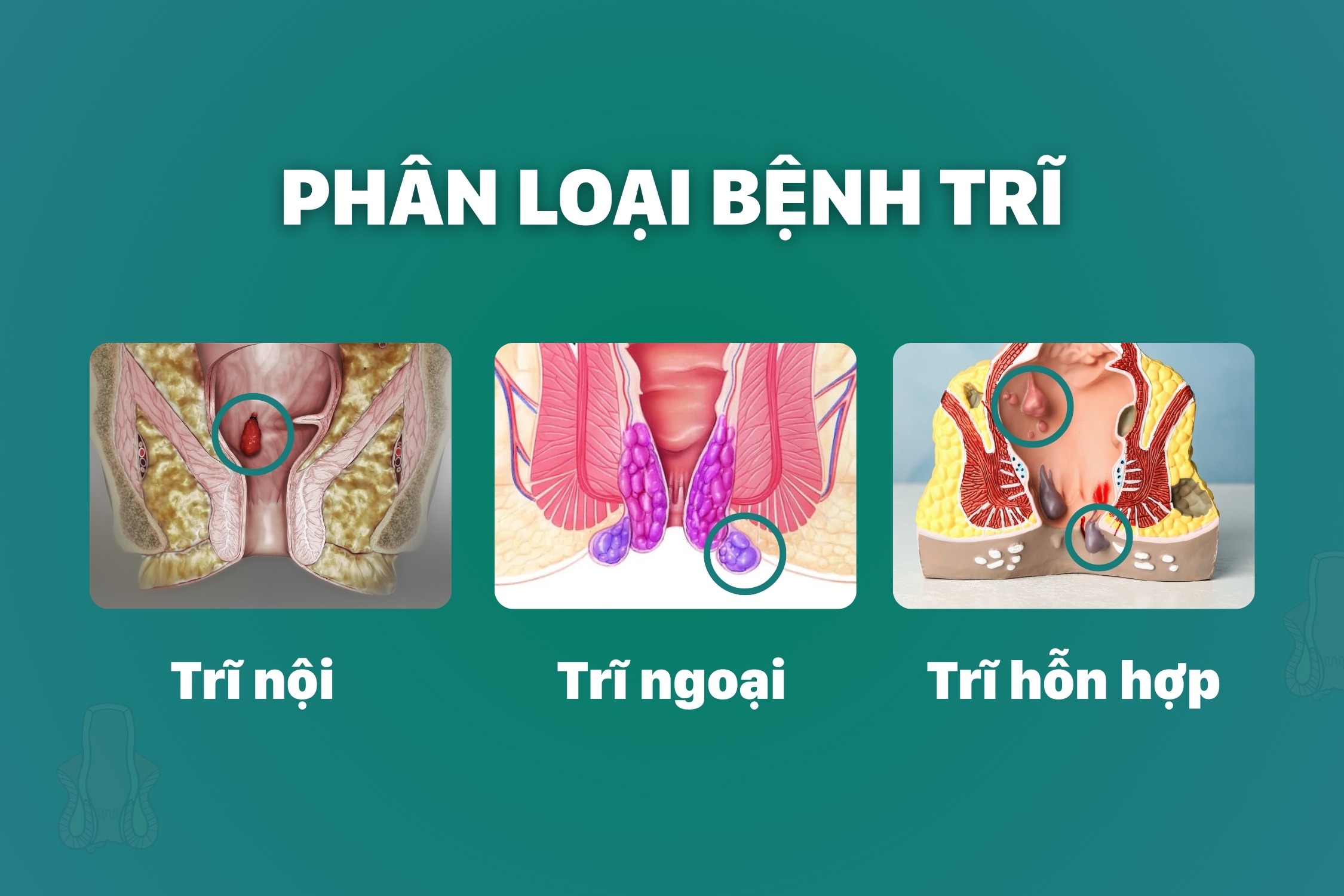
The clinical signs of external hemorrhoids are often readily identifiable by visual inspection. However, these manifestations may be confused with prolapsed internal hemorrhoids or other anorectal conditions such as anal skin tags, anal fissures, perianal abscess, or rectal prolapse.
Therefore, it is essential for patients to recognize early symptoms and potential complications of external hemorrhoids in order to seek timely medical evaluation and appropriate management.
What are external hemorrhoids?
Hemorrhoidal disease is the most common anorectal disorder in Vietnam, affecting approximately 35–50% of the population, according to the Vietnam Society of Coloproctology. Although not typically life threatening, it can significantly impair daily activities, mental well being, and work productivity.
External hemorrhoids develop as a result of excessive dilation of the venous plexus at the anal verge. In other words, they arise from increased pressure within the veins of the lower rectum and anus. Under sustained pressure, these veins become engorged, may bleed, and can protrude externally.
Differentiating internal and external hemorrhoids
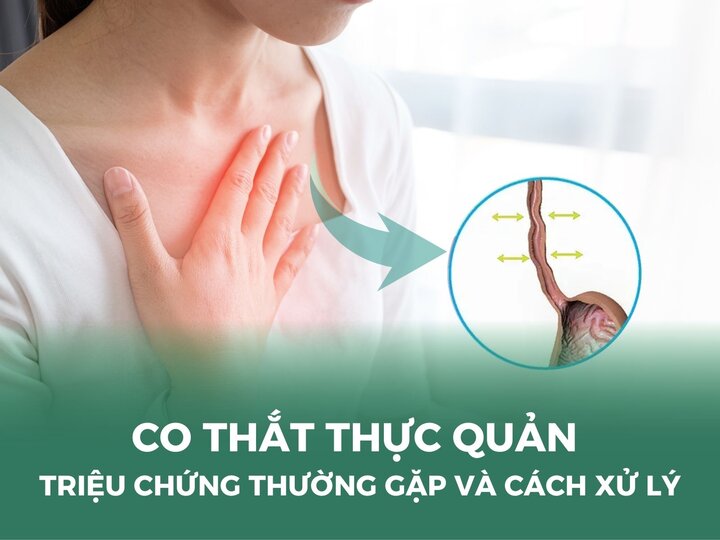
From an anatomical perspective, hemorrhoidal disease is classified into internal hemorrhoids, external hemorrhoids, and mixed hemorrhoids based on the dentate line within the anal canal:
- Internal hemorrhoids: These originate above the dentate line (the serrated anatomical boundary between the rectal mucosa and the anal canal epithelium). Because they are located within the rectum, early stage internal hemorrhoids are not visible externally and are often detected only when patients present with painless rectal bleeding during defecation. As the disease progresses, the hemorrhoidal tissue may prolapse through the anal canal during bowel movements.
- External hemorrhoids: These develop below the dentate line and are located beneath the perianal skin. External hemorrhoids are easily visible and palpable. They are more likely to cause pain, burning, and discomfort due to direct exposure to external factors such as clothing and prolonged sitting.
- Mixed hemorrhoids: This condition involves both internal and external hemorrhoids, with lesions located both above and below the dentate line, covered by mucosa and skin. When multiple hemorrhoidal masses coalesce circumferentially, they may form what is known as a circumferential (ring) hemorrhoid.
Clinical signs of external hemorrhoids
The clinical manifestations of external hemorrhoids may vary depending on disease severity. Common signs and symptoms include:
Mild external hemorrhoids:
- Passage of bright red blood during defecation
- Sensation of incomplete evacuation or rectal fullness
- Anal pain or burning, occurring during and after bowel movements, or persistent dull discomfort throughout the day, especially when sitting
- Prolapse of a small hemorrhoidal mass after defecation
- Perianal or rectal itching (pruritus ani)
Severe external hemorrhoids:
- Presence of perianal tissue resembling skin tags or enlarged masses, reddish in color and rich in vascular supply
- Persistent burning sensation in the anal region
- Markedly enlarged hemorrhoidal masses, often with a bluish purple discoloration
- Thrombosed external hemorrhoids causing severe pain, with a risk of rupture upon friction or pressure
It can be observed that the clinical manifestations of external hemorrhoids may overlap with other anorectal conditions such as anal skin tags, anal fissures, perianal abscess, rectal prolapse, and even colorectal malignancy, making misdiagnosis relatively common.
Therefore, experts strongly recommend that at the onset of any abnormal symptoms in the anorectal region, patients should promptly seek evaluation at a reputable healthcare facility. Consultation with a specialist is essential to establish an accurate differential diagnosis and ensure appropriate, condition specific management.
Reader may also be interested in:
- Stages of external hemorrhoids – when should you seek medical care?
- What are external hemorrhoids? What is the most effective and safe approach to the management of external hemorrhoids?
- Etiology of external hemorrhoids and effective preventive strategies
Patients are strongly advised not to delay medical care or self medicate with topical agents or unverified traditional remedies, as this may lead to disease progression, complicate treatment, and potentially result in serious, even life threatening complications.
How serious are the complications of external hemorrhoids?
In the early stage, external hemorrhoids are typically small, resembling a pea sized lesion. However, over time, they may enlarge into prominent masses, associated with pruritus, pain, and bleeding, particularly in cases of thrombosis.
If not detected early and managed appropriately, external hemorrhoids can lead to several potentially serious complications, including:
- Anemia and sepsis: Early manifestations of hemorrhoidal disease often include mild rectal bleeding, which may be overlooked as blood is minimal and mixed with stool or seen on toilet paper. Over time, persistent or heavy bleeding sometimes occurring as spurting can lead to chronic blood loss, resulting in fatigue, dizziness, and anemia. In cases complicated by perianal abscess, bacteria and toxins may enter the bloodstream, potentially causing sepsis, a life threatening condition.
- Thrombosed external hemorrhoids: Formation of blood clots within the hemorrhoidal vessels leads to firm, tense, bluish perianal masses, causing significant pain and impaired local blood circulation.
- Strangulated hemorrhoids: Enlarged hemorrhoidal masses may become trapped at the anal verge, obstructing defecation and causing severe pain, especially during bowel movements or physical activity. Prolonged strangulation can result in fissuring, bleeding, and secondary infection.
- Anal sphincter dysfunction: Chronic inflammation and mechanical obstruction may impair sphincter function, leading to difficulty in defecation or even fecal incontinence in severe cases.
- Hemorrhoidal necrosis: Persistent inflammation and infection can extend to surrounding tissues, potentially leading to anorectal abscess formation and tissue necrosis.
- Gynecological infections in women: Due to the anatomical proximity between the anus and female genital tract, infection from hemorrhoidal lesions may spread, increasing the risk of gynecological infections—particularly concerning in pregnant women, where both maternal and fetal health may be affected.
- Perianal dermatological conditions: Continuous mucous discharge from prolapsed hemorrhoids can irritate the surrounding skin, leading to dermatitis and chronic skin disorders.
When should patients with external hemorrhoids seek medical attention?
As outlined above, if not appropriately and promptly treated, external hemorrhoids may progressively worsen and lead to serious complications, potentially affecting overall health and quality of life.
Therefore, patients are advised to seek evaluation at a reputable healthcare facility and consult a specialist as soon as they experience abnormal symptoms, including:
- Anal pain, burning sensation, itching, or persistent moisture
- Difficulty during defecation and rectal bleeding
- Signs of anemia such as fatigue, dizziness, or weakness
In cases of mild external hemorrhoids, physicians typically recommend conservative management, including pharmacological therapy combined with dietary and lifestyle modifications to achieve optimal clinical outcomes.
- Increase intake of fruits and vegetables to provide adequate dietary fiber and support gastrointestinal function.
- Consume iron rich foods to prevent anemia associated with chronic hemorrhoidal bleeding.
- Limit fried and high fat foods, processed products, and avoid spicy foods, tea, coffee, stimulants, and alcohol.
- Maintain regular physical activity, exercising approximately 30–60 minutes per day.
- Avoid heavy lifting to reduce intra abdominal pressure.
- Do not strain excessively during defecation and avoid delaying bowel movements.
- Use a soft cushion or a specialized hemorrhoid cushion when sitting for prolonged periods.
Commonly indicated conservative (medical) treatment options include:
- Topical agents containing hydrocortisone or witch hazel extract to reduce inflammation, pruritus, and local irritation.
- Bowel regulating medications, including agents for constipation or diarrhea, along with venoactive drugs that enhance venous tone, strengthen vascular walls, and provide anti inflammatory effects.
- Rectal suppositories and ointments, applied locally to protect the hemorrhoidal mucosa and facilitate smoother stool passage.
- Analgesics such as ibuprofen, acetaminophen, or aspirin for pain relief (to be used under medical supervision).
- Cold compresses applied to the anal region using ice wrapped in a soft cloth to alleviate swelling and pain.
- Hypertonic saline ice packs, particularly useful in cases of thrombosed external hemorrhoids to reduce edema and discomfort.
Indications for surgical management of external hemorrhoids
Patients with advanced external hemorrhoids (stage 3 and stage 4) presenting with complications such as infection, significant edema, large hemorrhoidal masses, thrombosis causing acute vascular obstruction, profuse bleeding, severe pain, persistent discharge, or ulceration are typically indicated for surgical intervention.
Common treatment modalities include sclerotherapy, thermal coagulation, rubber band ligation, hemorrhoidectomy, and stapled hemorrhoidopexy (Longo procedure), aiming for definitive management.
However, the choice of procedure should be determined by a qualified specialist, based on comprehensive assessment of disease stage, severity of complications, and the patient’s overall clinical condition.
Hemorrhoidectomy in general, including surgery for external hemorrhoids, carries certain risks, such as:
- Intraoperative or postoperative bleeding
- Anal stenosis, which may be temporary or permanent
- Surgical site infection
- Fecal or urinary incontinence
Therefore, patients are strongly advised to undergo evaluation and surgical treatment at reputable healthcare facilities with experienced specialists, in order to minimize complications and reduce the risk of recurrence.
Hong Ngoc General Hospital – A trusted destination for hemorrhoid diagnosis and treatment in Hanoi
The Center for Gastrointestinal, Colorectal, and Pelvic Floor Surgery at Hong Ngoc General Hospital is a reputable medical facility widely chosen by patients for the management of hemorrhoidal disease. The center has successfully treated numerous cases of advanced hemorrhoids (stages 3 and 4) and associated complications, offering:
- Leading colorectal and anorectal specialists: Including Assoc. Prof. Dr. Nguyen Xuan Hung – Former Director of the Colorectal and Pelvic Floor Surgery Center, Viet Duc University Hospital; Vice President of the Vietnam Society of Coloproctology; Member of the French Society for Colorectal and Anal Diseases; Dr. Pham Van Cuong (MD, PhD, Specialist II) – Nearly 40 years of experience; Member of the Vietnam Society of Endoscopic and General Surgery; Dr. Cu Trung Kien (MD, MSc) – Advanced training in gastrointestinal surgery in Hong Kong; Former physician at Bach Mai Hospital; Deputy Head of the Department of Gastrointestinal Surgery, Hong Ngoc General Hospital; Dr. Bach Phuc Huy (MD, Specialist I) – Over 15 years of experience; Head of the Gastrointestinal Surgery Unit, Hong Ngoc – Phuc Truong Minh.
- Advanced surgical techniques: Application of modern hemorrhoid treatment technologies, including radiofrequency ablation, stapled hemorrhoidopexy (PPH), and Longo procedure.
- Painless hemorrhoid surgery: Comprehensive perioperative pain management (pre intra and postoperative) developed by Dr. Nguyen Thi Thu Ba (MD, MSc), with advanced residency training in France. A highly qualified anesthesia team ensures continuous intraoperative monitoring.
- Proactive pain prevention strategy: Rigorous pre anesthetic assessment, continuous intraoperative monitoring, and early pain control before symptom onset.
- 24/7 patient care support: Dedicated medical staff providing attentive care throughout hospitalization.
- Modern inpatient facilities: Spacious, clean environment with full amenities comparable to international hospital hospitality standards.

For detailed consultation, please contact:
Specialist appointment hotline: 0911 908 856Hemorrhoid surgery consultation hotline: 0949 646 556
Note: The information provided by Hong Ngoc General Hospital is for reference purposes only and does not replace professional medical diagnosis or treatment. Patients should not self medicate. For accurate evaluation of medical conditions, it is essential to visit reputable healthcare facilities for direct examination, diagnosis, and appropriate treatment planning by qualified physicians.
Follow the official fanpage of Hong Ngoc General Hospital for more useful health information and attractive healthcare programs.