The effectiveness of treatment depends on timely intervention according to each stage of the condition. What are the stages of disc herniation? Let us explore to enable accurate diagnosis and appropriate management at each stage.
What is a disc herniation?
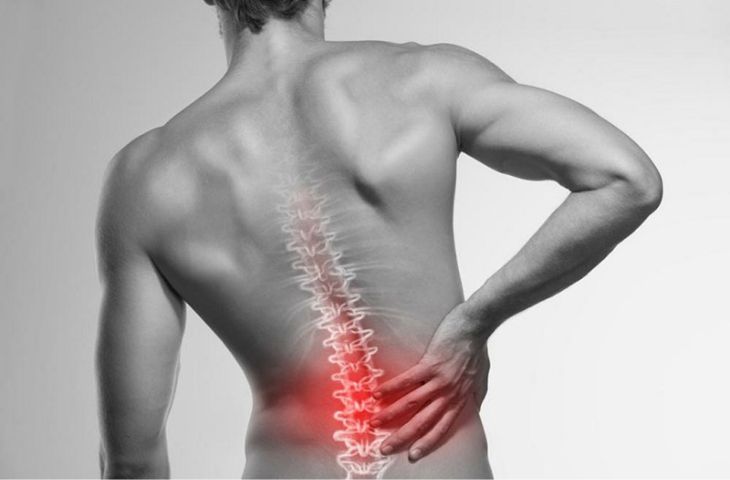
A disc herniation is a condition in which the nucleus pulposus protrudes beyond its normal position through the annulus fibrosus, compressing the spinal canal or adjacent nerve roots and causing spinal pain.
Disc herniation can occur at any level of the spine; however, it is most commonly seen in the cervical and lumbar regions, as these areas are most affected by daily activities and mechanical stress.
Types of disc herniation
Disc herniation can be classified based on anatomical location and the degree of neural compression.
By location:
- Posterior disc herniation: The most common type. Patients often present with back pain, discomfort, and numbness due to compression of nerve roots or the spinal cord.
- Anterior disc herniation: Typically asymptomatic, as the herniated disc does not compress neural structures.
- Intravertebral (Schmorl’s node): Occurs when disc material herniates into the vertebral body through the endplate.
Based on neural and spinal cord compression
Disc herniation can also be classified according to the degree and location of neural involvement:
- Central disc herniation: The nucleus pulposus protrudes centrally, directly compressing the spinal cord. Patients may experience persistent numbness in the extremities. This is the most severe form, as significant spinal cord compression can lead to loss of motor function and impaired bladder and bowel control.
- Paracentral disc herniation: The herniated disc compresses both the spinal cord and adjacent nerve roots, resulting in mixed neurological symptoms.
- Radicular (lateral) disc herniation: The disc compresses nerve roots on either the left or right side, typically causing unilateral symptoms such as pain, numbness, or weakness.
Stages of disc herniation
Disc herniation typically progresses through four stages:
Stage I: Early disc degeneration. This stage is characterized by initial deformation of the nucleus pulposus, with small fissures developing in the posterior annulus fibrosus. The nucleus begins to indent into these weakened areas. These changes are usually detectable only on specialized imaging, while standard imaging and clinical symptoms may remain unremarkable.
Stage II: Disc protrusion. The nucleus pulposus bulges toward a weakened portion of the annulus fibrosus, where multiple fissures and tears become more pronounced, although the outer layer remains intact. There is a reduction in intervertebral disc height, and the disc begins to protrude, particularly posteriorly. Imaging studies reveal clearer structural abnormalities, while clinically, patients may experience localized low back pain. In some cases, mild nerve root irritation may occur.

Stage III: Disc herniation. At this stage, the annulus fibrosus is completely ruptured, allowing the nucleus pulposus and other disc materials to protrude beyond the intervertebral space, forming a true herniation. Imaging may show herniated disc material with or without rupture of the posterior longitudinal ligament. Clinically, radicular syndrome becomes evident and can be classified into three levels:
- Nerve root irritation
- Nerve root compression with partial conduction preserved
- Complete loss of nerve conduction
Stage IV: Advanced degeneration (discarthrosis)The nucleus pulposus becomes deformed and fibrotic, while the annulus fibrosus is severely disrupted with multiple tears. There is a marked reduction in disc height, leading to secondary spinal canal stenosis, facet joint degeneration, and osteophyte formation along vertebral margins. Clinically, patients often present with chronic, recurrent low back pain and may develop severe radicular symptoms due to foraminal narrowing caused by secondary bony changes.
In clinical practice, disc pathology does not always progress sequentially through these stages. Disease progression may accelerate abruptly due to internal or external factors, particularly trauma or excessive mechanical loading. In some cases, severe disc degeneration may lead to spinal stiffness without overt disc herniation.
Important considerations in disc herniation
More than 90% of patients with low back pain and sciatica caused by disc herniation can be managed conservatively, while only approximately 5–10% require surgical intervention.
Patients with disc herniation should follow these recommendations:
- Activity modification: During the acute phase, patients are advised to rest in bed, preferably in a supine position on a firm surface, with support placed under the knees to slightly flex the hips and knees, thereby reducing intradiscal pressure. Patients may also adopt any position that provides maximal pain relief. Bed rest is typically recommended for 5–7 days, and in some cases may extend up to two weeks or longer depending on symptom severity.
- Psychological support: Physicians should clearly explain the purpose and importance of immobilization to ensure patient adherence. Proper and timely rest can prevent worsening of the herniation, reduce disc protrusion, and facilitate tissue healing. In some cases, small or early herniations may partially regress.
- Additional measures: While maintaining appropriate rest, patients may combine other supportive treatments such as heat therapy, gentle traction, massage, acupressure, spinal manipulation, acupuncture, physical therapy, and pharmacological management. Treatment should be individualized based on the patient’s condition.
From the second to third week onward, patients may begin gentle mobilization and perform light exercises in the supine position under medical supervision. The exercise regimen should follow these principles:
- Avoid postures and movements that generate high, sudden, or uneven mechanical loading
- Avoid excessive lumbar flexion, torsion, or shear forces; do not bend forward to lift heavy objects or carry loads asymmetrically. Instead, use the lower limbs (“squat” technique) and maintain proper spinal alignment at all times
- Avoid sitting or lying on the floor, as rising requires excessive spinal strain
- When getting out of bed, roll to the side, lower the legs, and then sit up; avoid abrupt straight sit ups
- Cough or sneeze in a seated position; hair washing should be performed in a supine or supported position during treatment
- Limit prolonged standing or sitting in a fixed posture
- Avoid walking long distances, running, or engaging in sports during treatment and for 3–6 months afterward
Physical therapy should be incorporated, including modalities such as spinal traction, electrical stimulation, laser therapy, and shockwave therapy, combined with specialized corrective exercises to help reposition the nucleus pulposus.
Additionally, patients should maintain a balanced diet rich in vegetables and essential nutrients, including vitamin D and B complex, to support musculoskeletal health.
After stabilization, patients can typically resume normal daily activities within 3–6 months.
Reader may also be interested in:
- What is disc degeneration? Causes, symptoms, and treatment options
- Lumbar spondylolisthesis: causes, symptoms and treatment options
When undergoing diagnosis and treatment for disc herniation at the Department of Rheumatology and Orthopedics, Hong Ngoc General Hospital, patients benefit from high quality healthcare services in Hanoi:
- Experienced and highly qualified medical team: Physicians with extensive expertise, trained and practiced at leading institutions such as Bach Mai Hospital, Viet Duc Hospital, and Royal North Shore Hospital (Australia)
- Advanced medical equipment imported from the United States: Including the SIGNA Prime MRI system, 128 slice CT scanner, Hologic bone densitometry system, and Logiq P7 musculoskeletal ultrasound, enabling high resolution imaging and early detection of musculoskeletal lesions
- Integrated rehabilitation approach: Combining physical therapy with advanced German therapeutic devices and specialized Austrian manual techniques to relieve pain and restore mobility effectively
- Personalized follow up plans: With proactive appointment scheduling for each patient
- Modern and comfortable facilities: Featuring free WiFi, cafés, and restaurants
- Weekend services available: Without additional charges
- Efficient insurance processing: Ensuring optimal patient benefits
Treatment of disc herniation at Hong Ngoc General Hospital helps rapidly alleviate pain, improve underlying pathology, and restore function without compromising patients’ overall health and quality of life.
Note: The information provided in this article by Hong Ngoc General Hospital is for reference purposes only and does not replace professional medical diagnosis or treatment. Patients should not self medicate. For accurate diagnosis and appropriate management, individuals are advised to visit a healthcare facility for direct examination, diagnosis, and consultation with qualified physicians.
Follow the official fanpage of Hong Ngoc General Hospital for more health updates and useful information:https://www.facebook.com/BenhvienHongNgoc