Stroke can lead to severe consequences for patients, including long-term disability and even death. Understanding stroke and its underlying risk factors is essential for effective prevention and for minimizing the devastating outcomes associated with this condition.
What is stroke?
Stroke, also known as a cerebrovascular accident, is a medical emergency that occurs when the blood supply to the brain is disrupted or significantly reduced, resulting in inadequate oxygen and nutrient delivery to brain tissue. When the brain is deprived of sufficient blood flow and oxygen, brain cells begin to die within minutes, leading to potentially severe neurological damage. Stroke is one of the leading causes of mortality and long-term disability worldwide.
There are two main types of stroke:
- Ischemic stroke: This is the most common type, accounting for approximately 80–85% of all cases. It occurs when an artery supplying blood to the brain becomes blocked, typically due to a blood clot or atherosclerotic plaque. As a result, the affected area of the brain is deprived of blood flow, leading to ischemia and subsequent brain tissue damage.
- Hemorrhagic stroke: This type occurs when a blood vessel within the brain ruptures, causing bleeding into or around the brain. The most common causes include rupture of weakened blood vessels, often associated with uncontrolled hypertension or vascular abnormalities.
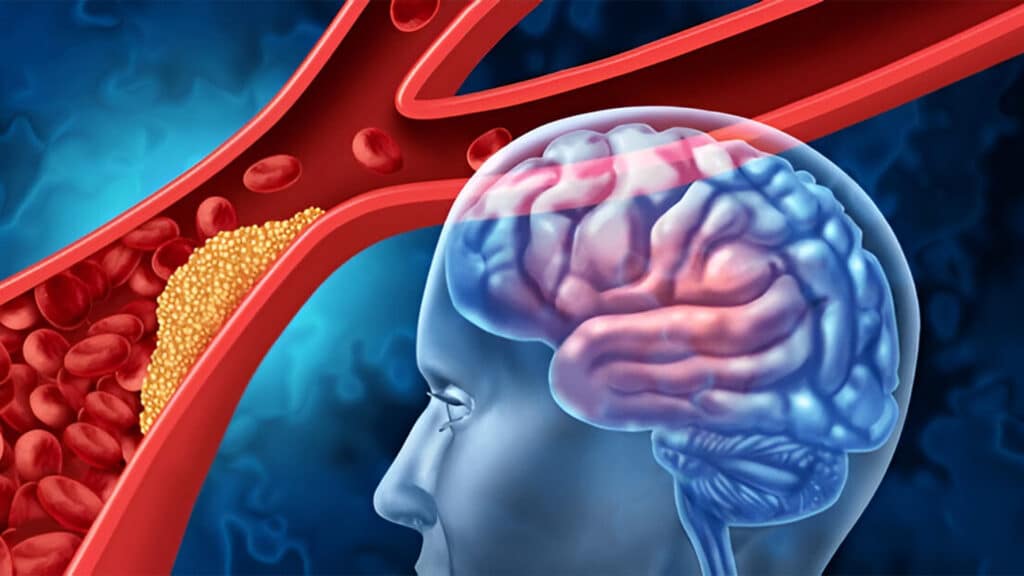
Risk factors for stroke
Several risk factors are associated with stroke. While some are non-modifiable, others can be effectively managed or controlled. The following are some of the most common risk factors:
- Hypertension: High blood pressure is one of the most significant risk factors for stroke. Persistent hypertension increases pressure on arterial walls, leading to vascular damage and promoting arterial narrowing or obstruction.
- Diabetes mellitus: Individuals with diabetes have a significantly higher risk of stroke compared with the general population. Chronically elevated blood glucose levels can damage blood vessels and contribute to cerebrovascular injury.
- Dyslipidemia: Elevated levels of cholesterol and blood lipids can accelerate atherosclerosis, leading to arterial narrowing or blockage and increasing the risk of stroke.
- Smoking: Tobacco use and exposure to secondhand smoke substantially increase the risk of stroke. Harmful chemicals in cigarette smoke damage blood vessels and promote thrombosis and vascular obstruction.
- Family history: A family history of stroke, particularly among first-degree relatives such as parents or siblings, may increase an individual's susceptibility to the condition.
- Age: The risk of stroke increases with advancing age. Individuals over the age of 55 are generally at higher risk.
- Cardiovascular disease: Conditions such as coronary artery disease and previous myocardial infarction are associated with an increased risk of stroke.
- Obesity: Excess body weight and obesity contribute to stroke risk by negatively affecting the circulatory system and increasing the likelihood of other risk factors such as hypertension and diabetes.
- Prolonged diarrhea: Persistent diarrhea may lead to dehydration and electrolyte imbalance, which can increase the risk of cerebrovascular complications.
To reduce the risk of stroke, it is essential to manage and modify controllable risk factors. These include maintaining optimal blood pressure, effectively controlling diabetes and cholesterol levels, quitting smoking, maintaining a healthy body weight, and adopting an overall healthy lifestyle.
Symptoms of stroke
The clinical manifestations of stroke can vary depending on the location and extent of brain injury. The following are some of the most common symptoms associated with stroke:
Loss of mobility or impaired movement
Patients may experience partial or complete loss of motor function, leading to difficulty walking, standing, or in severe cases, complete paralysis.
Loss of sensation or numbness
A portion of the body may become numb or lose sensation. This typically affects one side of the body, such as numbness or paralysis of the face, arm, or leg.

Speech and language impairment
Patients may experience difficulty speaking or understanding language, a condition known as aphasia. This can significantly impair communication or make it impossible.
Visual disturbances
Stroke may lead to partial or complete loss of vision. Patients may experience blurred vision, reduced visual acuity, or difficulty seeing with one or both eyes.
Sudden severe headache and nausea
Stroke, particularly hemorrhagic stroke, may present with a sudden and severe headache, often accompanied by nausea or vomiting. The headache can be intense and debilitating.
Loss of balance and coordination
Patients may have difficulty maintaining balance, walking, or standing steadily due to impaired coordination.
In addition, other symptoms may include shortness of breath, memory impairment, mood changes, reduced sensory perception, and difficulty performing daily activities.
Reader may also be interested in:
- What is cerebral blood circulation? 7 simple ways to improve cerebral blood circulation that anyone can do
- Impaired blood circulation and serious underlying cardiovascular disease
Importantly, these symptoms often occur suddenly. If any signs or symptoms of stroke are suspected, emergency medical services should be contacted immediately, or the patient should be transported to the nearest hospital for urgent medical evaluation and treatment.
Diagnosis of stroke
Accurate diagnosis of stroke requires prompt clinical evaluation and appropriate medical investigations. The following are some commonly used methods to diagnose stroke:
- Clinical examination: The physician performs a comprehensive clinical assessment to evaluate the signs and symptoms suggestive of stroke. This includes reviewing the patient’s medical history, current symptoms, and potential risk factors.
- Neurological assessment: A series of neurological tests are conducted to evaluate brain function, including assessments of sensory perception, vision, motor function, coordination, and reflexes.
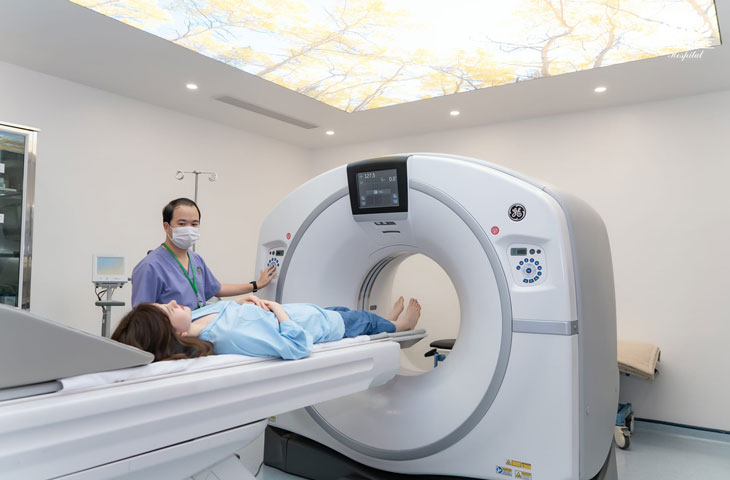
- Computed tomography (CT) scan of the brain: Brain CT imaging is commonly used to assess brain structure and detect lesions. It is particularly useful for determining whether the stroke is caused by a blood clot or intracranial hemorrhage.
- Magnetic resonance imaging (MRI) of the brain: MRI provides more detailed images of brain tissue and can accurately identify the location and extent of brain injury resulting from stroke.
- Blood tests: Laboratory blood tests are performed to evaluate various parameters, including blood glucose levels, coagulation profile, and other potential risk factors.
- Electrocardiography (ECG): ECG is used to assess the electrical activity of the heart and detect cardiac rhythm abnormalities that may contribute to stroke risk.
Additional diagnostic modalities, such as Doppler ultrasound, angiography, and electroencephalography (EEG), may also be utilized depending on the patient’s clinical condition and individual risk factors.
Treatment of stroke
The management of stroke requires immediate medical intervention and depends on the type of stroke as well as the patient’s overall clinical condition. The following are some commonly used treatment approaches:
Treatment of ischemic stroke
- Antithrombotic therapy: In cases of stroke caused by arterial occlusion, antithrombotic medications may be administered. These include antiplatelet agents such as aspirin and clopidogrel, as well as intravenous thrombolytic therapy (e.g., alteplase) to dissolve the blood clot and restore cerebral blood flow.
- Surgical intervention: In certain cases, surgical procedures may be performed to remove the obstructing clot or atherosclerotic plaque responsible for arterial blockage.
Treatment of hemorrhagic stroke
- Intracranial pressure management: In cases of hemorrhagic stroke, controlling intracranial pressure is critically important. This involves careful monitoring and regulation of blood pressure, ensuring adequate rest, and maintaining appropriate supportive care to facilitate stable breathing and cerebral perfusion.
- Surgical intervention: In certain cases, surgery may be required to control intracranial bleeding and remove accumulated blood clots within the brain.
In addition, following emergency treatment, neurological recovery and the management of brain injury represent essential components of comprehensive stroke care. Physicians may recommend rehabilitation therapy, lifestyle modifications, and pharmacological treatment to control underlying risk factors such as hypertension and diabetes mellitus.
Most importantly, when stroke is suspected, the patient should be transported to a medical facility as quickly as possible for urgent evaluation and treatment. Time is critical in minimizing brain damage and improving the chances of functional recovery.
Stroke prevention
Preventing stroke plays a crucial role in protecting brain health and maintaining a healthy circulatory system. The following are several recommended measures to help reduce the risk of stroke:
Blood pressure control: Hypertension is a major risk factor for stroke. Maintaining blood pressure within a healthy range and following medical guidance for blood pressure management are essential to reduce vascular stress.
Blood glucose control: For individuals with diabetes, maintaining stable blood glucose levels is critical in lowering the risk of stroke. Patients should adhere to dietary recommendations and undergo regular blood glucose monitoring as advised by their physicians.
Limit smoking and alcohol consumption: Tobacco use and excessive alcohol intake can significantly increase the risk of stroke. Smoking cessation and limiting alcohol consumption are strongly recommended.
Maintain a healthy lifestyle: Adopting a balanced and nutrient-rich diet, engaging in regular physical activity, maintaining a healthy body weight, and managing stress are important measures for stroke prevention.
Cholesterol management: Elevated cholesterol levels can contribute to atherosclerosis and increase the risk of stroke. A heart-healthy diet, reduced intake of high-fat and high-cholesterol foods, and appropriate lipid-lowering therapy when necessary can help control cholesterol levels.
Screening and management of related conditions: Medical conditions such as cardiovascular disease, arterial disorders, and peripheral vascular disease may increase stroke risk. Early detection and appropriate treatment of these conditions are essential for effective stroke prevention.
Regular health check-ups: Periodic medical examinations, including monitoring blood pressure, blood glucose, cholesterol, and other key health indicators, can help identify risk factors early and enable timely intervention.
In addition, understanding stroke risk factors and participating in health education and counseling programs can help individuals and their families improve awareness of stroke prevention and management.
Note: The information provided above is for general reference only and does not replace professional medical advice. If you experience any symptoms or have concerns related to stroke, you should seek prompt evaluation and treatment at a specialized medical facility.
The cardiology department at Hong Ngoc General Hospital is a trusted destination for cardiovascular care. With a team of highly qualified physicians and modern medical equipment, the department is capable of accurately diagnosing stroke and providing the most appropriate and effective treatment strategies, while offering dedicated consultation and personalized care for each patient.
Register here to receive consultation and schedule an examination with cardiology specialists at Hong Ngoc General Hospital:
Note: The information provided in articles published by Hong Ngoc General Hospital is for reference purposes only and does not replace professional medical diagnosis or treatment. Patients should not self-medicate without medical supervision. To obtain an accurate diagnosis and appropriate treatment plan, individuals should visit a medical facility for direct evaluation and consultation with a qualified physician.
Follow the official fanpage of Hong Ngoc General Hospital for more useful health information.