Sleep apnea syndrome not only impairs sleep quality but also poses significant risks to overall health. Understanding its causes, potential complications, and at-risk populations is essential for early prevention and timely intervention.
Causes of sleep apnea syndrome
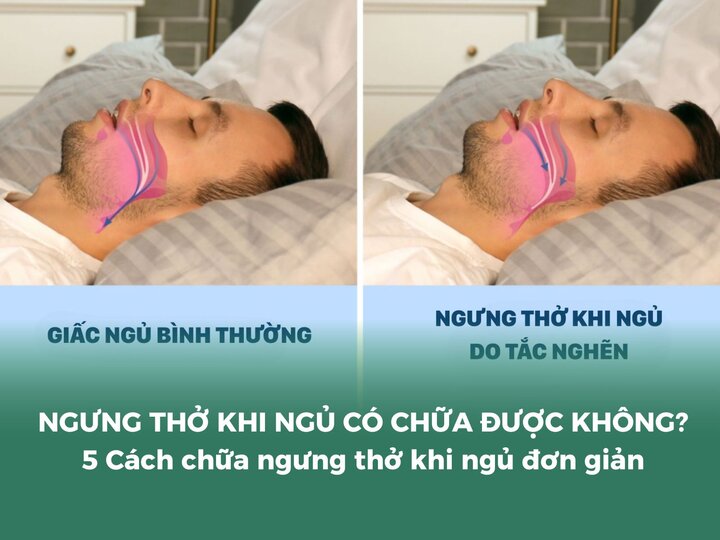
Sleep apnea is a condition characterized by collapse of the upper airway during sleep, leading to partial or complete interruption of airflow into the lungs, resulting in respiratory events including apnea and/or hypopnea.
The etiology of this syndrome is multifactorial and varies depending on the specific subtype. The principal contributing factors include the following:
Upper airway obstruction
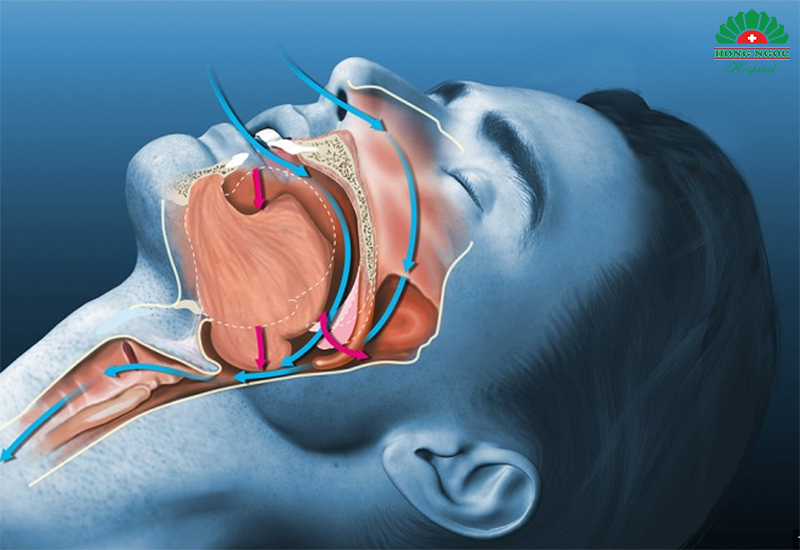
This is the leading cause of obstructive sleep apnea, accounting for approximately 80 to 90 percent of cases. During sleep, relaxation of the pharyngeal muscles leads to posterior displacement of the tongue and collapse of the pharyngeal walls, resulting in partial or complete airway obstruction and subsequent episodes of apnea or hypopnea.
Overweight and obesity
This is another common contributing factor. In individuals with excess body weight, adipose tissue accumulates around the neck and pharyngeal region, increasing extrinsic pressure on the airway and making it more prone to narrowing or collapse during sleep.
Anatomical abnormalities
Structural abnormalities of the upper airway, such as tonsillar hypertrophy, mandibular hypoplasia, macroglossia, or a deviated nasal septum, may also contribute to the development of sleep apnea.
Central nervous system dysfunction
Impaired central respiratory control occurs when the brain fails to transmit appropriate signals to regulate breathing rhythm, leading to disrupted respiratory patterns during sleep. This mechanism is more commonly observed in individuals with underlying neurological or cardiovascular disorders.
Unhealthy lifestyle habits
Lifestyle factors such as excessive alcohol consumption, cigarette smoking, use of sedative medications, irregular sleep patterns, and sleep deprivation may reduce respiratory muscle tone and increase the risk of sleep apnea.
High-risk populations for sleep apnea
Sleep apnea can occur in individuals of all ages; however, certain populations are at significantly higher risk, including:
Middle-aged and older adults
Advancing age is associated with reduced pharyngeal muscle tone, increasing the likelihood of upper airway collapse and disrupted breathing during sleep.
Male sex
Men are approximately two to three times more likely to develop sleep apnea than women, particularly during middle age.
Overweight and obese individuals
As previously noted, excess body weight contributes to fat accumulation around the neck, which can obstruct the upper airway. A higher body mass index is strongly correlated with an increased risk of sleep apnea.

Individuals with underlying medical conditions
Patients with comorbidities such as hypertension, diabetes mellitus, and cardiovascular disease are closely associated with an increased risk of sleep apnea.
Family history
Genetic predisposition plays a role in sleep apnea. Individuals with first-degree relatives affected by the condition, including parents, siblings, or children, have approximately a twofold higher risk compared to the general population. This may be related to shared anthropometric characteristics, upper airway anatomy, lifestyle habits, and other risk factors.
Children
Pediatric populations may also be at risk of sleep apnea. In children, the condition is commonly associated with adenotonsillar hypertrophy.
Warning signs and symptoms of sleep apnea
The most recognizable symptoms of sleep apnea include loud snoring, bruxism, witnessed apneic episodes, and episodes of choking or gasping during sleep. Patients may also experience frequent nocturnal awakenings and gastroesophageal reflux.
In addition, individuals with sleep apnea commonly present with excessive daytime sleepiness, morning headaches, and persistent fatigue throughout the day.
Furthermore, patients may exhibit reduced alertness, impaired motor coordination, neurocognitive dysfunction, and in some cases, sexual dysfunction.
When these symptoms are present, individuals should seek evaluation by a respiratory specialist for accurate diagnosis and appropriate, effective management.
Serious complications of sleep apnea syndrome
If not detected and treated early, sleep apnea syndrome can lead to a range of serious health complications, including:
Cardiovascular complications
Recurrent episodes of hypoxemia during sleep place excessive strain on the cardiovascular system. Over time, this may contribute to the development of hypertension, cardiac arrhythmias, myocardial infarction, and an increased risk of sudden cardiac death.
Metabolic disturbances
Individuals with sleep apnea syndrome are at increased risk of insulin resistance, type 2 diabetes mellitus, and dyslipidemia.
Cognitive and psychological impairment
Sleep fragmentation and chronic sleep deprivation associated with sleep apnea can lead to memory impairment, reduced concentration, and diminished cognitive performance. In addition, patients are more susceptible to mood disorders, including depression and anxiety.
Reduced quality of life
Poor sleep quality contributes to excessive daytime sleepiness, persistent fatigue, and impaired concentration, ultimately reducing work productivity and daily functioning. Furthermore, daytime drowsiness increases the risk of traffic accidents and occupational injuries.
Sexual dysfunction
Sleep apnea may adversely affect sexual health, with affected individuals having a higher risk of erectile dysfunction compared to the general population.
Why is early diagnosis important?
Sleep apnea is associated with multiple serious complications but can be effectively managed if detected at an early stage. Therefore, seeking specialist evaluation as soon as symptoms are recognized is essential.
However, clinical symptoms alone are insufficient for a definitive diagnosis. Objective diagnostic methods are required to accurately assess disease severity. Respiratory polygraphy is considered the gold standard for the diagnosis of sleep apnea.
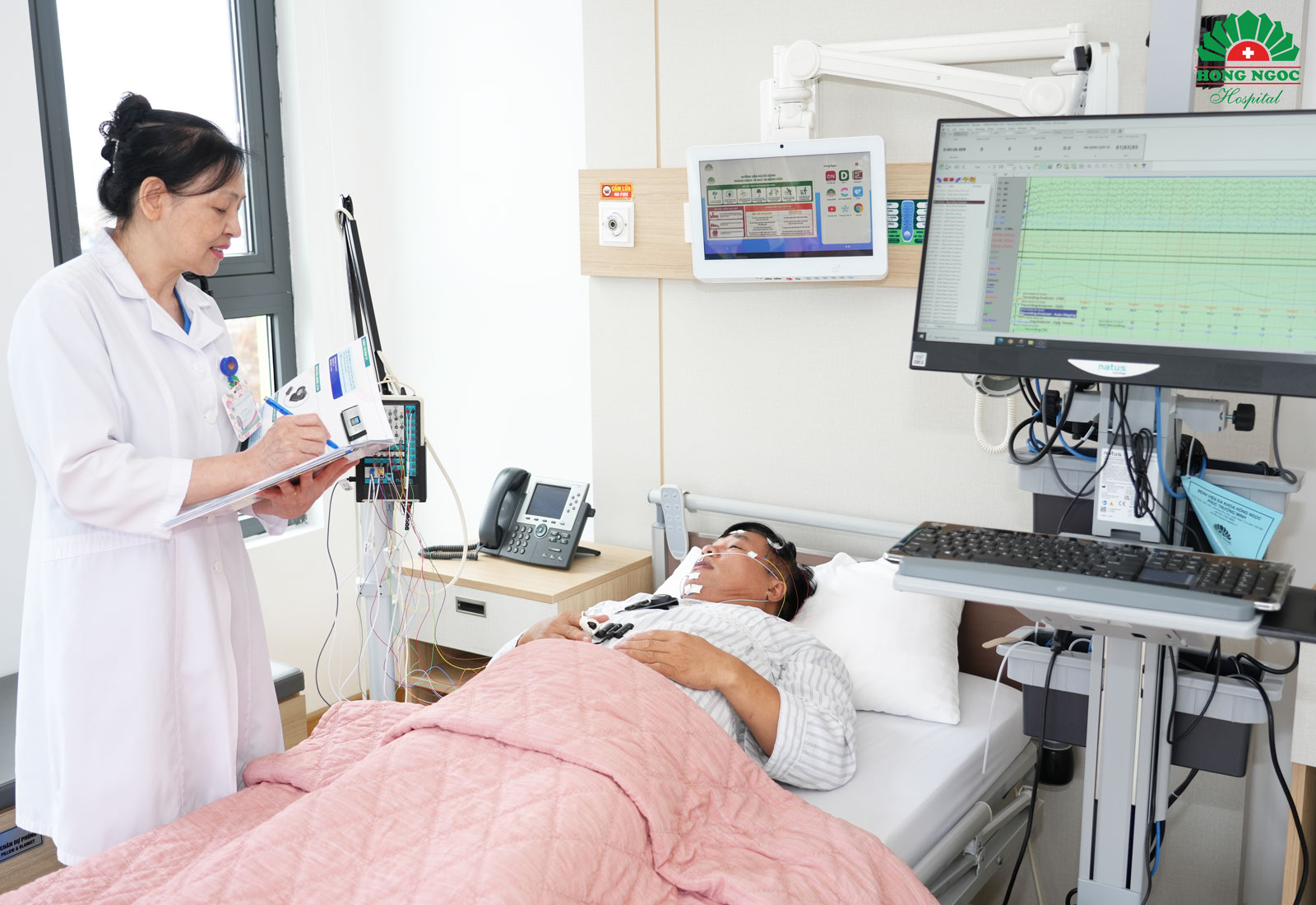
Respiratory polygraphy enables continuous monitoring of respiratory parameters during sleep, including the frequency and duration of apneic events, thereby allowing accurate classification of disease severity and supporting clinicians in selecting the most appropriate, individualized treatment strategy.
Hong Ngoc General Hospital is a trusted medical institution for the diagnosis and management of sleep apnea. The hospital is equipped with advanced respiratory polygraphy systems, ensuring high diagnostic accuracy. Notably, patients are evaluated and treated directly by experienced respiratory specialists, many of whom have previously worked at leading institutions such as Bach Mai Hospital and the National Lung Hospital, with personalized treatment protocols tailored to each case.
Reader may also be interested in:
- Sleep apnea: definition, clinical significance, etiology, and recognizable symptoms
- Obstructive sleep apnea: warning signs and treatment approaches
- Can sleep apnea be treated? Five simple home-based approaches to manage sleep apnea
Proactive screening with respiratory polygraphy facilitates early detection and timely intervention. Restorative sleep is fundamental to cardiovascular health and overall quality of life.
Department of Respiratory Medicine – Hong Ngoc General Hospital
No. 8 Chau Van Liem Street, Tu Liem Ward, Hanoi
No. 55 Yen Ninh Street, Ba Dinh Ward, Hanoi
Hotline: 0947 616 006