The clinical signs of internal hemorrhoids are often subtle and not easily recognized, making management more challenging compared to external hemorrhoids. Therefore, it is essential for patients to be aware of the early warning signs of internal hemorrhoids in order to seek timely and appropriate treatment.
What are internal hemorrhoids?
Internal hemorrhoids are characterized by the excessive dilation and enlargement of the venous plexus within the anorectal region, located below the dentate line. Over time, these hemorrhoidal cushions progressively increase in size and may prolapse outside the anal canal.
Internal hemorrhoids are often more difficult to diagnose than external hemorrhoids due to their deeper location within the anal canal. Many patients only become aware of the condition once the hemorrhoids have enlarged and symptoms such as rectal bleeding during defecation or prolapse begin to appear.
Typical signs of internal hemorrhoids
Compared to external hemorrhoids, internal hemorrhoids are less likely to cause severe pain. Instead, they present with more characteristic but often subtle clinical features, including:
- Increased mucous discharge from the anal canal
- Patients may not experience pain initially, even in the presence of rectal bleeding. However, excessive straining during defecation can cause mucosal injury to the hemorrhoidal tissue and anal canal, leading to inflammation, irritation, and pruritus ani particularly in individuals with excessive mucous secretion
- A persistent sensation of incomplete evacuation after defecation
In early stages, internal hemorrhoids are difficult to detect due to their location within the anal canal and the absence of visible or palpable masses. Over time, hemorrhoidal tissue may partially prolapse, especially during straining, with the following characteristics:
- Small in size (approximately pea-sized)
- Soft, elastic consistency, with a pinkish-red or skin-like coloration
- The prolapsed hemorrhoid may spontaneously reduce back into the anal canal
A patient may have multiple hemorrhoidal cushions, which can contribute to anal itching and the sensation of perianal lumps.
Grades of internal hemorrhoids
Based on the degree of hemorrhoidal prolapse and clinical presentation, internal hemorrhoids are classified into four grades, each with corresponding symptoms:
Grade I internal hemorrhoids:
- Mild rectal bleeding during defecation; blood is typically noted on the stool or toilet paper (intermittent in frequency)
- Burning sensation or discomfort during bowel movements
- Anal pruritus involving the anorectal region
- Chronic constipation
Grade II internal hemorrhoids:
- Increased rectal bleeding; blood may drip or even spurt during defecation
- Anal pain and burning sensation during bowel movements
- Anal itching and discomfort
- Notably, a small prolapsing mass may appear during defecation, which represents the hemorrhoidal tissue and typically reduces spontaneously afterward
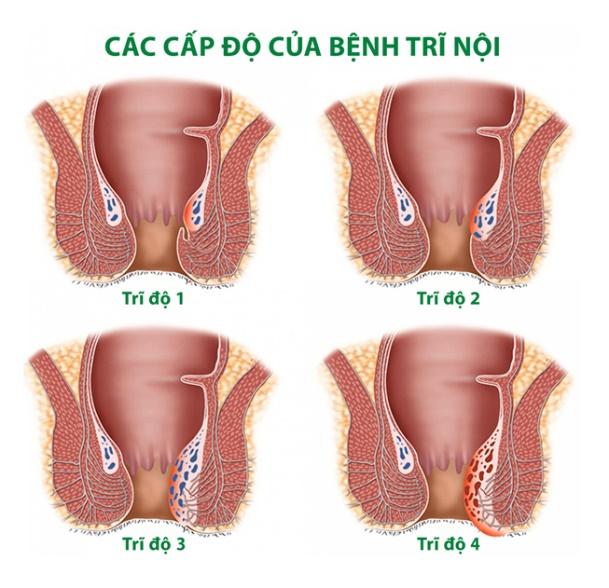
Grade III and IV internal hemorrhoids
Grade III internal hemorrhoids:
- Reduced rectal bleeding, which may lead patients to mistakenly assume spontaneous resolution, resulting in delayed medical evaluation and missing the final stage where conservative treatment may still be effective
- Prolapsed hemorrhoidal tissue that does not reduce spontaneously and requires manual repositioning
- Persistent anal pain and burning sensation, even without defecation; patients may have difficulty sitting due to pressure on the prolapsed hemorrhoids
Grade IV internal hemorrhoids:
- Irreducible prolapse of hemorrhoidal tissue, present even without defecation and not amenable to manual reduction
- Severe pain and significant bleeding during both movement and rest
According to medical experts, internal hemorrhoids and other anorectal conditions such as anal skin tags, anal fissures, perianal abscesses, rectal prolapse, and even rectal cancer may present with similar clinical features and are therefore easily misdiagnosed.
For this reason, patients presenting with any abnormal anorectal symptoms should seek prompt evaluation at reputable healthcare facilities. Assessment by a specialist is essential for accurate differential diagnosis and appropriate management from the early stages.
Reader may also be interested in:
- How are internal hemorrhoids classified? Treatment according to each grade
- Prolapsed hemorrhoids: beware of serious complications if not treated promptly
Patients are strongly advised not to delay care due to embarrassment or to self-medicate with topical agents or traditional remedies, as this may lead to disease progression, complicate treatment, and potentially result in serious, life-threatening complications.
Complications of internal hemorrhoids
If early signs of internal hemorrhoids are overlooked, the condition may progress and lead to serious complications, including:
- Anal fissures: Occur when enlarged hemorrhoidal tissue causes tears in the anal mucosa, resulting in severe pain and increasing the risk of secondary infection
- Infection of hemorrhoidal tissue: Large hemorrhoids may be subject to friction and irritation, predisposing to infection. Common presentations include inflammation of hemorrhoidal papillae, fissure-associated inflammation, diffuse hemorrhoidal inflammation, and perianal dermatitis
- Strangulated hemorrhoids: This complication arises when prolapsed hemorrhoids become trapped within the anal canal, leading to partial or complete obstruction. Patients may experience significant difficulty with defecation. If not promptly managed, this condition can progress to ulceration, infection, or necrosis
- Hemorrhoidal necrosis: May result from untreated infection, strangulation, or vascular thrombosis of the hemorrhoidal tissue. Necrosis can extend to surrounding anorectal structures if not treated in a timely and appropriate manner
- Sepsis: Severe infection originating from hemorrhoidal tissue may lead to systemic infection (sepsis), a life-threatening condition requiring urgent medical intervention
- Colorectal malignancy (differential consideration): Chronic anorectal inflammation and long-standing symptoms may mask or be mistaken for colorectal cancer. Therefore, thorough evaluation is essential to exclude malignancy in patients with persistent or atypical symptoms
- Clinical recommendation: Early diagnosis and appropriate management are critical to prevent complications. Patients with suspected hemorrhoidal disease should seek prompt evaluation by a specialist rather than delaying care or self-medicating.

In addition, internal hemorrhoids may lead to other serious complications and adverse outcomes, including:
- Anal sphincter dysfunction: weakening of the sphincter muscles, resulting in impaired control of flatus and fecal continence
- Rupture of hemorrhoidal tissue: leading to acute bleeding and increased risk of infection
- Secondary complications: including anal cryptitis, anorectal fistula formation, and chronic anorectal pruritus or inflammation
- Thromboembolic events: migration of thrombus to the mesenteric circulation, potentially causing vascular obstruction or systemic infection (sepsis)
These complications highlight the importance of early diagnosis and appropriate management of internal hemorrhoidal disease.
When should patients seek medical evaluation for internal hemorrhoids?
As discussed above, internal hemorrhoids do not resolve spontaneously. Without timely and appropriate treatment, the condition may progressively worsen, leading to serious complications that can significantly impact health and, in severe cases, become life-threatening.
Importantly, several symptoms of internal hemorrhoids may overlap with those of more serious conditions, such as colorectal cancer or anal malignancies. Therefore, patients should remain vigilant for accompanying signs, including changes in bowel habits, stool color, and stool characteristics.
Patients are advised to seek prompt evaluation at a reputable healthcare facility and consult a specialist if any of the following symptoms occur:
- Presence of a protruding mass or tissue at the anal region
- Anal pain, burning sensation, pruritus, or persistent moisture
- Difficulty with defecation or straining
- Rectal bleeding during bowel movements
Early medical assessment is essential for accurate diagnosis, appropriate differentiation from other conditions, and timely initiation of effective treatment.
Diagnostic methods for internal hemorrhoids
To establish a diagnosis of internal hemorrhoids, physicians may utilize the following approaches:
- Digital rectal examination (DRE): The physician performs a manual examination using a gloved, lubricated finger inserted into the rectum to assess for the presence of hemorrhoidal tissue, sphincter tone, and other potential abnormalities.
- Endoscopic evaluation (anoscopy/proctoscopy): A flexible endoscopic instrument is introduced through the anal canal to directly visualize the rectum and anal canal, allowing accurate identification and assessment of internal hemorrhoids.
A trusted center for the diagnosis and treatment of internal hemorrhoids
The Center for Gastrointestinal, Colorectal and Pelvic Floor Surgery at Hong Ngoc General Hospital is a reputable medical facility widely trusted for the treatment of hemorrhoidal disease. The Center has successfully managed numerous cases of grade III–IV hemorrhoids and related complications, supported by a highly experienced team of specialists:
- Prof. Nguyen Xuan Hung, MD, PhD, People’s Physician – former Director of the Colorectal and Pelvic Floor Surgery Center at Viet Duc University Hospital; Vice President of the Vietnam Society of Colorectal and Anal Diseases; member of the French Society for the Treatment of Colorectal and Anal Diseases
- Dr. Pham Van Cuong, MD, PhD, Specialist Level II, Meritorious Physician – with nearly 40 years of experience; member of the Vietnam Society of Endoscopic Surgery and the Vietnam Society of Surgery
Hemorrhoid management with specialists ensures:
- Accurate diagnosis: avoiding misdiagnosis with rectal cancer, polyps, and other anorectal conditions
- Comprehensive treatment: approximately 50% of cases can be managed with medication and lifestyle modification, while 45% require only minimally invasive procedures
- Effective intervention: minimal tissue damage, rapid recovery, very low complication rates, with a success rate exceeding 95%
For further consultation, please contact:
- Hotline for appointments with Prof. Nguyen Xuan Hung: (+84) 911 908 856
- Hotline for hemorrhoid surgery consultation: (+84) 949 646 556
Register to receive information and consultation at:
- Center for Gastrointestinal, Colorectal and Pelvic Floor SurgeryHong Ngoc Phuc Truong Minh Hospital – 8 Chau Van Liem, Nam Tu Liem District, Hanoi
- Hong Ngoc General Hospital – 55 Yen Ninh, Ba Dinh District, Hanoi
Note: The information provided is for reference purposes only and does not replace professional medical diagnosis or treatment. Patients should visit reputable healthcare facilities for direct evaluation and appropriate treatment planning by qualified physicians.
Follow the official fanpage of Hong Ngoc General Hospital for more health information and updates.