Cardiovascular disease is one of the most dangerous medical conditions, with mortality rates ranking among the highest worldwide. What are the underlying causes of cardiovascular disease, and how can it be effectively prevented? These questions will be addressed in the scope of this article.
Adverse effects of cardiovascular disease
Adverse impacts of cardiovascular disease
Cardiovascular disease reflects pathological impairment of the heart and/or the blood vessels supplying the heart, resulting in reduced cardiac function and an inability to pump sufficient blood to meet the metabolic demands of other organs. Consequently, systemic organ perfusion is compromised, leading to progressive organ dysfunction and, if left untreated, eventual organ failure and death.
The clinical consequences vary depending on the specific type of cardiovascular disease and its severity. In mild cases, patients may experience symptoms such as dizziness, headache, and dyspnea, which significantly affect quality of life. Over time, without appropriate treatment, the disease may progress and lead to serious, life-threatening complications, including myocardial infarction and stroke.
According to multiple epidemiological reports, cardiovascular disease is the leading cause of death worldwide, accounting for a higher proportion of mortality than any other cause. In Vietnam, cardiovascular-related deaths accounted for approximately 31% of all deaths in 2016.
This highlights the critical need to raise public awareness of cardiovascular disease, including its adverse impacts, underlying causes, and effective preventive measures, in order to minimize the prevalence of cardiovascular-related conditions within the population.

Causes of cardiovascular disease
Cardiovascular disease can be classified into two main types:
Congenital heart disease
Congenital heart disease refers to structural abnormalities of the myocardium, cardiac valves, or cardiac chambers that develop during fetal life and persist after birth. When one or more cardiac structures are defective, normal cardiac function and hemodynamics are compromised. The clinical impact varies depending on the type and severity of the defect, ranging from minimal functional limitation to significant impairment of daily activities and overall quality of life.
Congenital heart disease is one of the most common congenital anomalies and represents a leading cause of mortality among congenital disorders in infants and young children. However, with advances in medical technology, many congenital cardiac defects can now be detected early through routine prenatal ultrasound examinations during pregnancy.
There are two main causes of congenital heart disease:
Genetic factors
Genetic predisposition is considered one of the most significant contributors to the development of congenital anomalies, particularly congenital heart defects. Children born into families in which one or both parents, or other close relatives, have congenital heart disease are at a higher risk of being affected. In certain cases, even when both parents are clinically unaffected, the presence of pathogenic genes in both individuals may still confer a high risk of congenital heart disease in their offspring.
Toxic exposure or maternal illness during pregnancy
During the first trimester of pregnancy, maternal infection with viruses such as rubella or herpes, or the presence of maternal systemic diseases including systemic lupus erythematosus and diabetes mellitus, significantly increases the risk of congenital anomalies in the fetus, particularly congenital heart defects.
In addition, pregnant women living in toxic environments or frequently exposed to ionizing radiation, such as X-rays, are at higher risk of gestational toxicity, which may adversely affect fetal development and increase the likelihood of congenital malformations.
Furthermore, maternal consumption of alcohol, tobacco, and other addictive substances, as well as the use of certain medications during pregnancy, is associated with a markedly increased risk of congenital defects in newborns, including congenital heart disease.

Acquired heart disease
Acquired heart disease refers to cardiovascular conditions that develop after birth and are not related to congenital heart defects. The underlying causes are most commonly associated with unhealthy lifestyle and dietary habits, including tobacco smoking, physical inactivity, chronic psychological stress, high intake of saturated fats, excessive alcohol consumption, obesity, high salt intake, diabetes mellitus, and elevated cholesterol levels. Acquired heart disease may also arise as a complication of certain chronic medical conditions.
These risk factors are particularly prevalent among men, especially in middle-aged populations, contributing to a higher incidence of acquired cardiovascular disease in this group.
However, in recent years, due to multiple contributing factors, the lifestyle and dietary habits of many young people have become increasingly unhealthy and poorly structured. This has led to a clear trend toward younger onset of cardiovascular disease. Notably, a growing number of individuals in their early twenties have already experienced myocardial infarction or stroke, conditions that were previously observed mainly in middle aged and elderly populations.
Common acquired cardiovascular diseases
Coronary artery disease is characterized by the accumulation of atherosclerotic plaques or cholesterol deposits along the arterial walls, leading to narrowing of the arterial lumen, reduced blood flow, and impaired delivery of oxygen and nutrients to tissues and organs throughout the body.
As these atherosclerotic plaques progressively thicken, cardiac function gradually deteriorates. Clinical manifestations are often nonspecific, and many patients experience only vague symptoms such as chest heaviness or exertional angina. In some cases, headache, dizziness, and dyspnea may also occur.
To ensure timely detection and effective management, regular health examinations are essential. Adopting a balanced, heart healthy diet and engaging in daily physical activity play a crucial role in strengthening cardiac function and maximizing prevention of coronary artery disease as well as other cardiovascular disorders.
Cerebrovascular accident, also known as stroke
A cerebrovascular accident, commonly referred to as stroke, occurs when cerebral blood circulation is interrupted or severely reduced, resulting in inadequate oxygen and nutrient supply to brain tissue. This leads to neuronal cell death and may cause severe, long term neurological sequelae or death in severe cases.
Reader may also be interested in:
- Cardiovascular diseases
- What is dyspnea? Causes of shortness of breath
- Is heavy breathing dangerous? Causes and treatment
Clinical subtypes of cerebrovascular accident include cerebral vasospasm, transient ischemic attack, cerebral infarction, intracerebral hemorrhage, and subarachnoid hemorrhage.
The clinical manifestations are often acute and pronounced, typically presenting with sudden severe headache, dizziness, unilateral limb weakness, altered consciousness, or coma.
There are two primary causes of this condition:
Hypertension
Individuals with hypertension are at a markedly increased risk of stroke, as persistently elevated blood pressure raises mechanical stress on the vascular walls, leading to arterial dilation and endothelial injury. In response, platelets and fibrin strands are recruited to repair damaged areas of atherosclerosis, which may inadvertently result in thrombus formation. These thrombi can migrate through the circulation to the cerebral vessels, causing vascular occlusion and subsequent cerebral infarction.
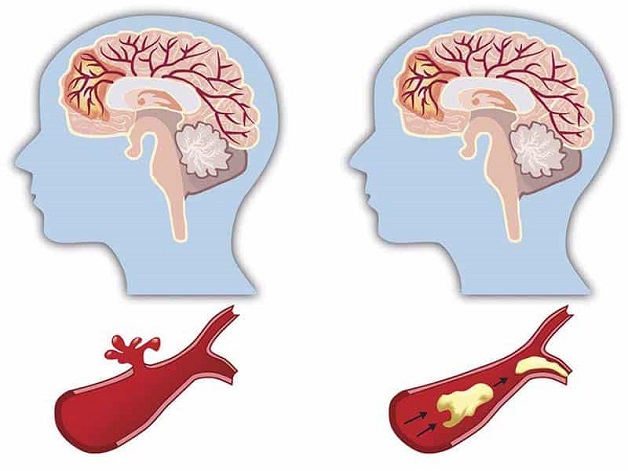
Atherosclerosis
Atherosclerosis leads to progressive narrowing of blood vessels, thereby impairing normal blood flow. When atherosclerotic plaques rupture or detach, they can give rise to thrombus formation, which may obstruct cerebral circulation and precipitate ischemic stroke.
To reduce the risk of cerebrovascular accidents, it is essential to maintain optimal blood pressure control and minimize the progression of atherosclerosis through a healthy, evidence based lifestyle and regular medical check ups.
Peripheral arterial disease (PAD) occurs when plaques composed of fat, cholesterol, calcium, and other substances accumulate within the arterial walls. Over time, these plaques harden, leading to progressive narrowing of the arteries and impaired blood flow.
Peripheral arterial occlusive disease includes two main forms:
Buerger disease (thromboangiitis obliterans)
This condition involves inflammation of all three layers of the arterial wall and typically occurs in young individuals under 40 years of age, particularly heavy tobacco users. The disease has a prolonged course, and up to 95 percent of patients may ultimately require limb amputation.
Atherosclerotic peripheral arterial disease
This form occurs primarily in individuals with hypertension and dyslipidemia, resulting from progressive atherosclerotic plaque formation that leads to arterial narrowing and occlusion.
Clinical manifestations of peripheral arterial disease are often nonspecific and easily overlooked. Typical symptoms include intermittent calf pain during walking that resolves quickly after 5 to 10 minutes of rest. In some cases, patients may experience limb discomfort, pale or cool skin, and the development of ulcers with delayed healing.
Post-rheumatic valvular heart disease is an autoimmune condition resulting from infection with Streptococcus beta-hemolyticus.
Following infection, the immune system produces antibodies to eliminate the pathogen. However, Streptococcus beta hemolyticus shares structural similarities with joint tissue and cardiac valve tissue. As a result, the antibodies fail to distinguish between the pathogen and host tissues, leading to autoimmune-mediated damage to the joints and heart valves. This process causes inflammation, valvular deformity, stenosis or regurgitation, and may ultimately result in heart failure.
The disease occurs more frequently in young women and is a complication of streptococcal pharyngitis. It typically progresses insidiously, with clinical manifestations including migratory polyarthritis, joint pain, carditis, fever, and the appearance of subcutaneous nodules.
Treatment is primarily based on antibiotic therapy to eradicate the underlying streptococcal infection and prevent further autoimmune damage.
Aortic dissection of the thoracic aorta
Thoracic aortic dissection is a condition in which the aorta, the main artery supplying blood to the body, becomes weakened and dilated, leading to a tear in the aortic wall. This tear allows blood to rapidly dissect between the layers of the aortic wall, causing massive internal bleeding and potentially resulting in rapid death.
This condition carries an extremely high mortality rate, reaching up to 95 percent even in the early stages. The primary underlying causes include uncontrolled hypertension, atherosclerosis of the aorta, and traumatic injury that predisposes to aortic weakening and subsequent dissection.
Cardiomyopathy
Cardiomyopathy occurs when the myocardium becomes weakened and is unable to pump an adequate volume of blood to meet the body’s metabolic demands. If not detected and treated promptly, the condition carries a high risk of sudden cardiac death.
The etiology of cardiomyopathy includes viral infections, particularly Coxsackie virus infection, exposure to certain medications or toxic chemicals, and endocrine disorders such as hyperthyroidism.
In the early stages, cardiomyopathy is often asymptomatic. As the disease progresses, patients may develop dyspnea, fatigue, dizziness, and peripheral edema, especially in the lower extremities.
Cardiomyopathy can be prevented to some extent through a healthy lifestyle and measures to strengthen the immune system. When symptoms such as persistent fatigue or shortness of breath occur, patients should seek medical evaluation at healthcare facilities and undergo specialized diagnostic investigations to enable early diagnosis and treatment, thereby minimizing severe complications.
For individuals with suspected symptoms or a confirmed diagnosis of heart disease, regular follow-up with a cardiology specialist is strongly recommended to monitor cardiovascular health, prevent adverse events, and ensure timely management of potential complications.
Register for a consultation with a cardiology specialist here:
Effective prevention of cardiovascular disease
To prevent and limit the progression of cardiovascular diseases, in addition to regular health check ups, individuals should engage in routine physical activity and maintain a healthy, well balanced lifestyle:
- Avoid smoking, refrain from alcohol consumption, and do not use stimulatory substances.
- Maintain a heart healthy diet by limiting unhealthy fats and sugars while ensuring adequate intake of all essential nutrients to support optimal health.
- Maintain a stable body weight, avoiding excessive or rapid weight gain and preventing obesity.
- Ensure adequate sleep and minimize prolonged stress and anxiety.
Note: The information provided in this article by Hong Ngoc General Hospital is for reference purposes only and is not intended to replace professional medical diagnosis or treatment. Patients should not self medicate under any circumstances. To accurately determine their medical condition, patients are advised to visit a hospital or healthcare facility for direct examination, diagnosis, and consultation with qualified physicians regarding an appropriate treatment plan.
Follow the official fanpage of Hong Ngoc General Hospital for additional useful health information.