Valvular heart disease is a common cardiovascular disorder observed in both neonates and adults. In this article, we provide a comprehensive overview of valvular heart disease, including its etiological factors, clinical manifestations, diagnostic evaluation, and contemporary therapeutic modalities for optimal disease management.
What is valvular heart disease?
Valvular heart disease refers to a pathological condition in which the functional integrity of one or more cardiac valves is impaired, resulting in abnormal cardiac hemodynamics and disrupted blood flow through the heart. If not detected early and managed appropriately, this condition can significantly reduce quality of life and, in advanced stages, may become life threatening.
Valvular heart disease may be congenital or acquired. In adults, acquired valvular disorders commonly arise from a variety of etiologies, including infectious diseases, degenerative changes, inflammatory conditions, or adverse lifestyle factors.
The cardiac valves, including the mitral valve, tricuspid valve, aortic valve, and pulmonary valve, are located at the outflow pathways of the four cardiac chambers. Their essential physiological role is to maintain unidirectional blood flow and prevent backward leakage. Each valve consists of leaflets, also known as cusps, that open and close during every cardiac cycle. When one or more valves fail to open completely, known as valvular stenosis, or fail to close properly, referred to as valvular regurgitation, normal intracardiac blood flow is compromised, leading to clinically significant valvular heart disease.
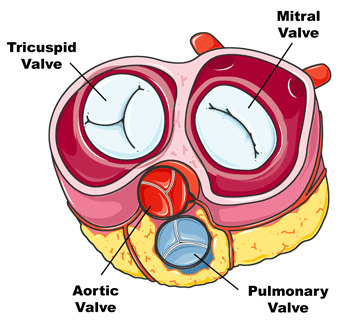
Common valvular heart diseases
There are numerous types of valvular heart disorders; below are the most commonly encountered conditions in clinical practice:
Valvular stenosis
Also referred to as aortic stenosis, this condition occurs when the aortic valve becomes narrowed, resulting in restricted blood flow from the left ventricle into the systemic circulation. It is one of the most prevalent forms of valvular heart disease encountered in clinical practice.
The primary underlying mechanism of aortic stenosis is progressive fibrotic and calcific deposition on the aortic valve leaflets, leading to leaflet thickening, reduced mobility, and valvular rigidity. Additional etiologies include congenital valvular malformations, inflammatory or infectious processes, age related degenerative changes, and atherosclerotic disease.
Valvular regurgitation
Also referred to as valve regurgitation, this condition occurs when a cardiac valve fails to close completely, allowing blood to leak backward from the chamber into which it was ejected to the preceding cardiac chamber.
Valvular regurgitation can compromise cardiac pumping efficiency, increase intracardiac volume overload, and, if left untreated, may lead to serious complications, including heart failure and other adverse cardiovascular outcomes.
Valvular regurgitation may arise from multiple etiologies, including:
- Congenital valvular abnormalities: Structural malformations or incomplete development of the cardiac valves present at birth may impair proper leaflet coaptation.
- Valvular injury or inflammation: Any form of structural damage, infective endocarditis, or inflammatory process affecting the valve apparatus can disrupt normal valve closure and result in regurgitant flow.
- Atherosclerotic disease: Progressive atherosclerosis may contribute to valvular thickening, reduced elasticity, and impaired leaflet mobility, thereby preventing complete valve closure.
- Myocardial dilation: Ventricular dilation can distort the valvular annulus and subvalvular apparatus, leading to inadequate leaflet coaptation and secondary functional regurgitation.
Mitral valve stenosis
Also referred to as mitral stenosis, this condition occurs when the mitral valve becomes narrowed, thereby restricting blood flow from the left atrium to the left ventricle. It is one of the most common forms of valvular heart disease encountered in clinical practice.
The primary underlying mechanism of mitral stenosis is fibrotic thickening and structural remodeling of the mitral valve leaflets, which results in leaflet rigidity and impaired opening and closure. Progressive narrowing of the valvular orifice reduces the effective valve area, thereby limiting blood flow from the left atrium into the left ventricle and leading to elevated left atrial pressure.
Valvular regurgitation
Also referred to as valvular insufficiency or valve incompetence, this condition occurs when a cardiac valve fails to close completely, allowing blood to flow backward from the chamber into which it was ejected to the preceding cardiac chamber. Valvular regurgitation can impair cardiac output and, if progressive, may lead to significant hemodynamic compromise and serious cardiovascular complications.
The primary underlying mechanism of valvular regurgitation is structural damage or functional impairment of the valve apparatus. Specific etiologies include:
- Congenital valvular abnormalities: In some individuals, the cardiac valves do not develop normally at birth, resulting in defective leaflet structure or inadequate coaptation.
- Infective endocarditis: Infection of the cardiac valves may cause leaflet destruction, perforation, or deformation, leading to incomplete valve closure.
- Valvular injury: Any structural damage affecting the valve leaflets, chordae tendineae, papillary muscles, or annulus can weaken the valvular apparatus and result in regurgitation.
- Other valvular disorders: Certain forms of valvular stenosis or structural deformation may alter normal valve mechanics and subsequently contribute to secondary valvular regurgitation.

Tricuspid regurgitation
This condition occurs when the tricuspid valve fails to close completely, resulting in backward blood flow from the right ventricle into the right atrium during systole.
Clinical manifestations may include fatigue, dyspnea, and signs of right atrial and right ventricular enlargement. In more advanced cases, patients may develop peripheral edema, hepatomegaly, and other features consistent with right sided heart failure.
Infective endocarditis
Also referred to as infective endocarditis, this condition is a serious infection involving the endocardial lining of the heart and the cardiac valves. It represents a life threatening disorder that may result in severe systemic and cardiovascular complications if not promptly diagnosed and treated.
Infective endocarditis typically develops when microorganisms, most commonly bacteria and less frequently viruses or fungi, enter the bloodstream and adhere to the surface of a cardiac valve or previously damaged endocardial tissue. Colonization and proliferation at these sites lead to the formation of vegetations and progressive valvular destruction.
Several risk factors increase susceptibility to infective endocarditis:
- Pre-existing valvular damage: Previously damaged or structurally abnormal valves, such as those affected by stenosis or regurgitation, provide a favorable substrate for microbial adherence and growth.
- Exposure to bacteremia: Situations associated with transient bacteremia, including dental procedures, invasive vascular interventions, or exposure to contaminated environments, may facilitate microbial seeding of the cardiac valves.
- Immunocompromised states: Individuals with impaired immune function, including those with immunodeficiency disorders, diabetes mellitus, substance use disorder involving intravenous drug use, or other systemic illnesses, are at increased risk of developing infective endocarditis.
Causes of valvular heart disease
Valvular heart disease can arise from various causes. Some of the most common include:
- Congenital valve abnormalities: Some individuals are born with structural defects of the heart valves. These may occur when a valve does not develop properly, has too few or too many leaflets, or has an abnormal structure or position.
- Infections: Bacteria or viruses may enter the bloodstream and infect the heart valves, leading to infective endocarditis. Such infections can originate from other parts of the body, including dental infections, pharyngitis, pneumonia, or urinary tract infections.
- Physical damage: Trauma or age related degeneration may weaken or damage the heart valves over time.
- Other systemic diseases: Certain conditions, such as rheumatic disease or pericardial inflammation, may also affect the heart valves and impair their function.
- Genetic factors: In some cases, hereditary predisposition may increase the risk of developing valvular heart disease.
Any structural abnormality or damage to the heart valves can lead to valvular dysfunction. Identifying the underlying cause and establishing an appropriate treatment plan requires thorough evaluation and consultation with a cardiology specialist.
Reader may also be interested in:
- 11 Warning signs of heart disease that require immediate medical attention
- Valvular regurgitation and therapeutic management
- Valvular stenosis: Clinical manifestations, etiologies, management, and prevention
Symptoms of valvular heart disease
Valvular heart disease can cause a range of symptoms depending on the type of valve affected and the severity of the damage. Common manifestations include:
Shortness of breath
Dyspnea is one of the hallmark symptoms of valvular heart disease. It may occur during physical exertion or even during routine daily activities such as climbing stairs. This symptom arises when the affected heart valve fails to function properly, leading to impaired blood flow through the heart and reduced oxygen delivery to the body.

Fatigue and reduced physical capacity
Valvular heart disease may cause persistent fatigue and decreased energy levels. When the heart cannot pump efficiently, the body receives insufficient blood and oxygen, leading to reduced stamina and diminished physical performance.
Irregular heartbeat
Some patients may experience cardiac rhythm disturbances, including tachycardia (rapid heart rate) or arrhythmia (irregular heartbeat).
Chest pain
Chest discomfort or pain may occur in valvular heart disease. This may result from valve stenosis or regurgitation, which increases pressure within the heart.
Cough and dry cough
Valvular dysfunction may lead to pulmonary congestion and fluid accumulation in the lungs, resulting in persistent coughing or dry cough accompanied by shortness of breath.
Edema and swelling
Severe valvular heart disease can cause fluid retention, leading to swelling in various parts of the body, such as the legs, arms, abdomen, or face. This occurs due to increased venous pressure and excess fluid accumulation.
Dizziness and fainting
Reduced blood and oxygen supply to the brain may lead to dizziness, lightheadedness, or episodes of syncope.
These symptoms may vary in frequency and severity depending on the specific valve disorder, the degree of valve damage, and the patient’s overall health condition.
Diagnosis of valvular heart disease
To accurately diagnose valvular heart disease, physicians perform a comprehensive clinical examination and may recommend specialized tests and imaging studies using advanced medical equipment. These evaluations help determine the exact condition and severity of valve damage, allowing doctors to select the most appropriate treatment strategy.
Some commonly used diagnostic methods and tests include:
- Medical history: The physician will collect detailed information about the patient’s medical history, including current symptoms, their onset, duration, and frequency. Patients may also be asked about any family history of cardiovascular disease.
- Clinical examination: A comprehensive physical examination will be performed, including cardiac auscultation, blood pressure measurement, and evaluation of other related signs and symptoms.
- Blood tests: Laboratory tests may include routine blood analysis, assessment of cardiac and hepatic function, and screening for markers of infection or inflammation.
- Cardiac function tests: Physicians may request tests to evaluate heart function, such as echocardiography to assess the structure and function of the heart valves; a stress test to evaluate cardiac performance during physical exertion; or electrocardiography (ECG) to record the electrical activity of the heart.
- Imaging studies: In some cases, imaging techniques such as magnetic resonance imaging (MRI) or computed tomography (CT) may be used to provide detailed visualization of the heart valves and surrounding cardiac structures.
- Cardiac catheterization: In more severe cases, physicians may perform cardiac catheterization, a procedure in which a thin catheter is inserted through a blood vessel to directly evaluate the heart valves and nearby blood vessels.
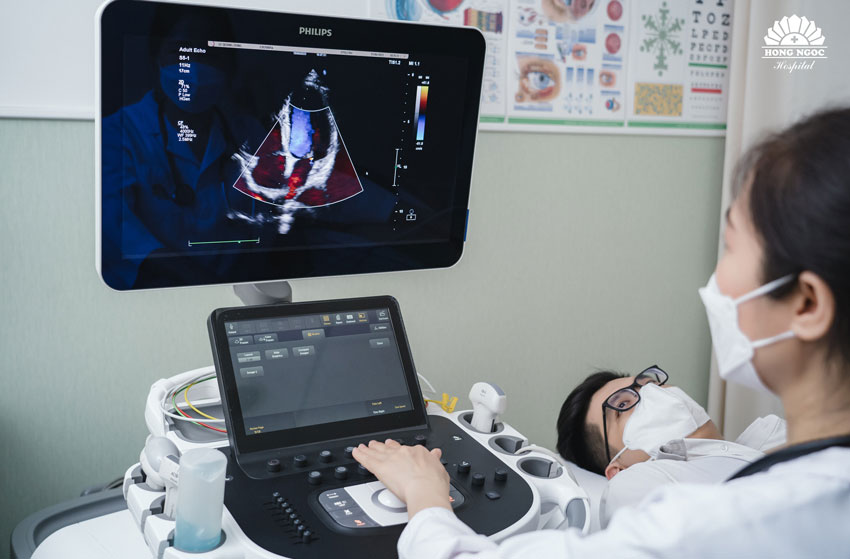
Treatment and management of valvular heart disease
Management of valvular heart disease may include both non-surgical and surgical approaches, depending on the severity of the condition and the specific valve involved.
Medication
Pharmacologic therapy is commonly used to manage symptoms and control disease progression. Different medications may be prescribed to relieve symptoms, regulate heart rhythm, and reduce the workload on the heart. These may include vasodilators, antibiotics (in cases of infection), antiarrhythmic drugs, and anticoagulants.
Heart valve replacement
In severe cases where the function of the heart valve cannot be restored, patients may be indicated for valve replacement surgery. This procedure involves removing the damaged valve and replacing it with either a mechanical prosthetic valve or a biological valve derived from donor tissue.
Heart valve repair
Valve repair surgery may be performed to correct conditions such as valve stenosis, regurgitation, or structural abnormalities. During the procedure, the surgeon may reshape the valve, reconstruct its structure, or repair the damaged components to restore normal valve function.
Control of risk factors
Patients with valvular heart disease should manage cardiovascular risk factors by maintaining a healthy lifestyle. This includes following a balanced diet, engaging in regular physical activity, maintaining a healthy weight, and limiting alcohol consumption and smoking. Adhering to medical advice is essential to maintain stable cardiovascular health.
Regular monitoring and ongoing treatment
Valvular heart disease requires continuous monitoring and long term management. Patients should undergo regular follow up examinations at reputable healthcare facilities to track disease progression, adjust medications when necessary, and monitor related health indicators such as blood pressure, blood glucose, and coagulation status.
The Cardiology Department at Hong Ngoc General Hospital is a trusted center for cardiovascular care. With a highly qualified team of cardiologists and modern medical equipment, the hospital provides early detection of valvular heart diseases and individualized treatment strategies for optimal patient outcomes.
Register for an examination and receive consultation from cardiology specialists here:
Note: The information provided in this article by Hong Ngoc General Hospital is for reference purposes only and does not replace professional medical diagnosis or treatment. Patients should not self-medicate. For an accurate assessment of their medical condition, individuals are advised to visit a healthcare facility for direct examination, diagnosis, and appropriate treatment planning by a qualified physician.
Follow the official fanpage of Hong Ngoc General Hospital HERE for more useful health information.